For patients undergoing total knee arthroplasty (TKA), restoring strength and mobility is only part of the recovery journey. One of the most overlooked aspects of early recovery is postural sway after knee replacement, a subtle yet powerful indicator of how well the body maintains balance and adapts to sudden changes. Many patients experience a higher fall risk after TKA, even when pain decreases and joint mobility improves, but why?
Traditionally, clinicians have attributed postoperative instability to “poor balance”, reduced proprioception, or insufficient muscle strength. While these factors matter, they only scratch the surface of a far more complex neuromuscular process.
A growing body of research shows that the pattern of a person’s postural sway, not just how much they sway, reveals critical information about their nervous system, adaptability, and ability to prevent falls. This is known as postural sway complexity, and it reflects the health and responsiveness of the neuromuscular system.
A recent study brings new clarity by demonstrating that the surgical technique used during TKA can significantly influence this complexity, impacting a patient’s ability to maintain stable, adaptive balance during the crucial first weeks of rehabilitation.
In this article, we explore why postural sway matters after knee replacement, what postural sway complexity reveals about fall risk, how different surgical techniques affect it, and what these findings mean for patients, surgeons, and rehabilitation professionals.
CONTENTS
1- What Is Postural Sway?
2- What Is Postural Sway Complexity? (Complex vs Simple Sway)
3- Study Design: How the Researchers Measured Postural Sway Complexity
4- Breakthrough: A New Link Between Surgical Technique and Neuromuscular Adaptability
5- FAQ: Postural Sway After Knee Replacement
6- Conclusion
7- Reference
1- What is Postural Sway?
Even when you feel like you are standing perfectly still, your body is never truly motionless. Instead, it constantly makes tiny, involuntary adjustments to maintain your center of mass over your base of support. These subtle movements are known as postural sway.

Postural sway results from the continuous interaction of multiple systems:
- Sensory systems: proprioception, vision, and vestibular input
- Neuromuscular control: the brain’s ability to interpret sensory information and produce corrective actions
- Musculoskeletal structures: joint mechanics, ligament integrity, and muscle activation
Together, they form a feedback loop that keeps you upright.
Why Postural Sway Matters
Postural sway is not a sign of weakness or instability. In fact, everyone sways, and this sway is essential for maintaining balance. It reflects how efficiently the body can detect changes, process information, and respond with precise muscular adjustments.
How Postural Sway Is Measured
Most commonly, postural sway is measured using center of pressure (CoP) data from a force plate. The CoP represents the point of contact beneath your feet where ground reaction forces act. By tracking this movement, clinicians and researchers can quantify how the body maintains postural control.
Traditional sway measurements include:
- Sway amplitude (how far you move)
- Sway velocity (how fast you move)
- Sway direction (front-back vs side-to-side patterns)
However, these measurements only describe the quantity of sway. They do not reveal the quality of the neuromuscular control system.
A Deeper Layer: The Pattern Behind the Sway
What truly matters is not just how much a person sways but how the sway pattern is organized over time. This organization reflects the health, adaptability, and responsiveness of the balance system.
This is where postural sway complexity becomes a powerful and sensitive marker, one that traditional balance metrics cannot capture.
2- What Is Postural Sway Complexity? (Complex vs Simple Sway)
While postural sway describes how much a person moves while standing still, postural sway complexity describes how the neuromuscular system organizes that movement over time. It is a measure of the adaptability, robustness, and responsiveness of the balance control system.
This distinction is crucial: two people may sway the same amount, but the pattern of their sway can reveal dramatically different levels of neuromuscular health.
Complex Sway: A Healthy, Adaptive System
A healthy postural control system generates sway that is rich, dynamic, and complex. To visualize this, imagine an experienced driver navigating a winding road. They make countless micro-adjustments:
- rapid,
- precise,
- and responsive to every subtle change.

These adjustments do not follow a rigid or predictable pattern, and that’s exactly what makes them effective. The system is highly adaptable, ready to react instantly to a bump, a sudden turn, or an unexpected obstacle.
In biomechanics, this adaptability appears as high sway complexity. It signals:
- strong communication between the body and the brain,
- a flexible neuromuscular system,
- efficient integration of sensory feedback,
- and the ability to recover from perturbations quickly.
High complexity is therefore considered a marker of a healthy balance system.
Simple Sway: A Fragile, Less Adaptive System
Now imagine a new driver learning to steer. Their corrections are:
- delayed,
- stiff,
- and inconsistent.
Their pattern becomes more rigid, more repetitive, or sometimes more random but not adaptive. This represents low sway complexity.
In the body, such simplicity often emerges after:
- surgery,
- injury,
- pain,
- fatigue,
- or neurological impairment.
A system with low complexity is less capable of responding to sudden changes, making it more vulnerable to slips, trips, missteps, and ultimately falls.
Low complexity =
❌ less adaptability
❌ less resilience
❌ higher fall risk
Understanding postural sway and its complexity requires precise, reliable measurements of the center of pressure. If you want to assess balance quality, not just sway amplitude, portable force plates can offer a deeper, more actionable view of a patient’s neuromuscular control.
K-Force Plates are portable, lightweight force plates designed to measure both static and dynamic balance across a wide range of tasks, from quiet stance to squats and other functional movements. They provide real-time CoP tracking, asymmetry analysis, and objective metrics that support both assessment and balance training.
Ideal for proprioception testing, neuromuscular evaluation, and rehabilitation progress tracking, K-Force Plates fit seamlessly into any clinical or field-based setting.
Why Complexity Matters After Knee Replacement
Following TKA, the neuromuscular system undergoes temporary and sometimes lasting disruptions. Pain, swelling, altered joint mechanics, and surgical trauma can all reduce the nervous system’s ability to coordinate balance.
Even if a patient appears stable in quiet standing, their sway complexity may tell a different story:
- A high-complexity sway suggests the system is adapting well.
- A low-complexity sway indicates fragility and a higher risk of destabilization.
This is why sway complexity is emerging as a critical predictor of fall risk after knee replacement, and why it provides far more information than traditional measures of sway amplitude or velocity.
This study is the first to ask: Does the specific surgical technique used in a knee replacement damage this healthy, complex balance system?
3- Study Design: How the Researchers Measured Postural Sway Complexity
To understand how surgical technique affects postural sway after knee replacement, the researchers designed a controlled, comparative study focusing on women undergoing total knee arthroplasty (TKA). Their goal was to determine whether the surgical approach influences the neuromuscular adaptability reflected in sway complexity.
Participants and Group Allocation
The research team recruited 20 women scheduled for knee replacement surgery and randomly assigned them to one of two widely used surgical approaches:
- Medial Parapatellar (PP) approach
- Mid-Vastus (MV) approach
To establish a benchmark for healthy balance patterns, the results from these surgical groups were compared with those of a control group of 11 healthy women with no history of knee pathology or neuromuscular impairment.
Measuring Postural Sway Complexity
Postural sway was assessed using center of pressure (CoP) data collected during quiet standing. This allowed researchers to analyze not only how much each participant swayed, but how the sway pattern evolved, the key to understanding sway complexity.
Measurements were taken at four timepoints:
- One day before surgery (baseline)
- Five days after surgery
- Two weeks after surgery
- One month after surgery
This timeline allowed the researchers to track both the immediate postoperative changes and the evolution of neuromuscular control during the early stages of recovery.
The Complexity Metric
To quantify the complexity of postural sway, the study used the α-exponent derived from Detrended Fluctuation Analysis (DFA), a validated nonlinear method often used in biomechanics to detect patterns, adaptability, and long-range correlations in physiological signals.
- Higher α values → more structured or predictable sway (lower complexity)
- Lower α values → richer, more adaptive sway (higher complexity)
This method is particularly sensitive to subtle changes in neuromuscular control that traditional balance metrics cannot detect.
Why This Design Matters
By comparing two surgical techniques across multiple recovery stages, and by using a nonlinear complexity metric, the study provides a unique window into how surgery affects the neurological foundations of balance, not just mechanical stability or strength.
4- Breakthrough: A New Link Between Surgical Technique and Neuromuscular Adaptability
The breakthrough here is linking a specific surgical choice to a sophisticated, underlying marker of neurological health. This study moves beyond the vague idea of “good” or “bad” balance. It provides hard data showing that how a surgeon operates can directly impact the brain’s ability to run its complex, adaptive balance program, which is critical for preventing falls.
The Results
The findings were clear. While both groups showed some loss of complexity right after surgery, a significant difference emerged over time.
- Patients in the Medial Parapatellar (PP) group showed a major, significant loss of postural complexity at the 2-week and 1-month marks. Their balance patterns became simpler and less healthy, diverging significantly from the healthy control group.
- Patients in the Mid-Vastus (MV) group did not show this significant loss. Their balance patterns remained much closer to those of the healthy control group, suggesting their underlying balance system was far less affected by the surgery.
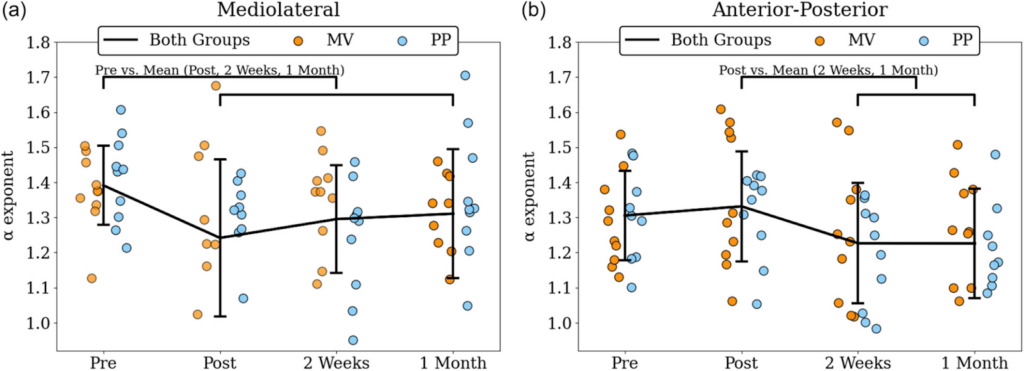
Figure 1. α exponent (the complexity metric) of CoP at the mediolateral (a) and the anterior-posterior (b) axis for both groups (black line), and separately for MV (orange dots) and for PP (blue dots) for all measured timepoints. Annotated brackets indicate the statistically significant contrasts. CoP, center of pressure; MV, mid-vastus; PP, parapatella.
What This Means for Patients, Surgeons & Rehabilitation Professionals
- For Patients: This study suggests that the way your knee replacement is performed could have a direct impact on your recovery and fall risk. The mid-vastus (MV) approach appears to be more effective at preserving the body’s natural, healthy, and complex balance system. This could mean a safer recovery with more stability and confidence during those crucial first weeks.
- For Surgeons: This research provides powerful evidence that the choice between the PP and MV techniques is not just about surgical access, but has measurable consequences for a patient’s neurological function and safety after they leave the operating room. For female TKA patients, the mid-vastus approach may offer a significant advantage in preserving the postural control system, potentially lowering the risk of postoperative falls.
- For Rehabilitation professionals: This study highlights the need to look beyond strength and range of motion after TKA. Postural sway complexity offers valuable insight into a patient’s neuromuscular adaptability, signaling how well they can respond to balance challenges. Early balance and perturbation training may help restore this adaptability, and patients who undergo the PP approach may require additional fall-prevention support in the first month. Ultimately, effective rehabilitation must focus not only on strength but on rebuilding the complexity and resilience of postural control.
5- FAQ: Postural Sway After Knee Replacement
What is postural sway after knee replacement?
Postural sway refers to the natural, continuous adjustments your body makes to stay upright. After knee replacement, these adjustments can change due to altered joint mechanics, swelling, pain, and temporary neuromuscular disruption, making sway patterns an important indicator of fall risk.
Why does fall risk increase after total knee replacement (TKA)?
Fall risk increases because TKA affects proprioception, muscle activation, and neuromuscular coordination. Even if a patient feels stable, their balance system may be less adaptable, especially if postural sway complexity decreases.
What is postural sway complexity?
It is the measure of how adaptive and flexible your balance control system is. A complex sway pattern indicates a healthy, resilient neuromuscular system. A simple, repetitive pattern signals fragility and a higher risk of losing balance.
How is postural sway measured?
Sway is typically measured using force plates, which track how your center of pressure (CoP) moves while you stand. Complexity is calculated using nonlinear methods like Detrended Fluctuation Analysis (DFA).
Does the surgical technique influence postural sway?
Yes. This study found that the Medial Parapatellar (PP) approach led to a significant loss of sway complexity during early recovery, while the Mid-Vastus (MV) approach preserved it far better. This suggests that surgical technique can affect neuromuscular adaptability.
Does lower sway complexity mean I’m more likely to fall?
Low complexity means the balance system is less adaptable to sudden changes, making slips, trips, or unexpected weight shifts more dangerous. While it’s not the only factor, it’s a strong indicator of increased fall risk after TKA.
Can rehabilitation improve postural sway complexity?
Yes. Balance training, perturbation exercises, proprioceptive work, and neuromuscular stimulation may help restore adaptability. Early monitoring and individualized rehab can be especially important for patients showing low complexity.
6- Conclusion
Postural sway after knee replacement is far more than a simple measure of stability; it is a window into the neuromuscular system’s ability to adapt, recover, and protect the body from falls. This study demonstrates that the quality of sway, particularly its complexity, is a sensitive marker of postoperative resilience that traditional balance assessments often overlook.
Most importantly, the research reveals that surgical technique matters. While both groups experienced short-term changes in balance, patients who underwent the Mid-Vastus (MV) approach preserved their postural sway complexity far better than those who received the Medial Parapatellar (PP) approach. This preservation of neuromuscular adaptability may translate into safer early mobility, fewer balance-related incidents, and greater confidence during recovery.
For patients, this means understanding that balance recovery extends beyond strength and mobility. For surgeons, it highlights the neurological implications of their technical approach. For rehabilitation professionals, it reinforces the need to evaluate and train the adaptive components of balance, not just force output or joint range.
As the field continues to embrace more nuanced, data-driven approaches to postoperative recovery, postural sway complexity is emerging as a powerful and insightful metric, one that may ultimately help reduce fall risk and improve outcomes for thousands of TKA patients.

