Manual therapy is widely used in physical therapy and rehabilitation to reduce pain, improve mobility and restore physical function. Based on hands-on techniques performed by trained clinicians, it includes joint mobilization, manipulation, soft tissue techniques, and other manual approaches commonly used in musculoskeletal care.
Today, manual therapy is integrated into the management of many conditions, including low back and neck pain, musculoskeletal disorders, sports injuries and post-operative rehabilitation. It is often used to decrease pain, improve movement, and help patients return to normal activity.
However, beyond its traditional image as a purely hands-on approach, the role of manual therapy has evolved. Advances in research and the growing importance of active rehabilitation have changed how healthcare professionals use it in daily practice.
What exactly is manual therapy? How does it work? Is it truly effective according to scientific evidence? And what is its role in modern, evidence-based rehabilitation?
This article explores the definition, mechanisms, and effectiveness of manual therapy, as well as its real place in contemporary physical therapy and rehabilitation.
CONTENTS
1- What Is Manual Therapy?
2- How Does Manual Therapy Work?
3- Is Manual Therapy Effective? What the Evidence Says
4- The Role of Manual Therapy in Modern Rehabilitation
5- Conclusion
6- FAQ: Answer Your Questions about Manual Therapy
7- References
1- What Is Manual Therapy?
According to the International Federation of Orthopaedic Manipulative Physical Therapists (IFOMPT), manual therapy is a specialized area of physical therapy dedicated to the management of neuromusculoskeletal disorders. It is based on clinical reasoning and uses highly specific treatment approaches, including manual techniques and therapeutic exercise.

This approach plays a central role in the management of musculoskeletal disorders. It is commonly used for back and neck pain, shoulder, knee, and ankle conditions, as well as during rehabilitation following injury or surgery.
Contrary to common misconceptions, hands-on treatment is not limited to joint manipulation. It includes a wide range of techniques such as:
- joint mobilization
- high-velocity low-amplitude manipulation
- soft tissue techniques
- specific stretching
- neurodynamic techniques
The goal is not only to act locally on a joint or muscle, but to improve overall movement, function and patient confidence in movement.
Today, manual therapy is rarely used as a standalone intervention. It is usually integrated into a broader rehabilitation strategy combining therapeutic exercise, strength training and patient education to achieve sustainable outcomes and promote long-term autonomy.
2- How Does Manual Therapy Work?
Manual therapy involves a range of hands-on techniques applied to joints, muscles and neural tissues to reduce pain, improve mobility and facilitate movement. It is commonly used in physical therapy to help patients move more comfortably and regain function.
For many years, the effects of manual techniques were explained primarily through a biomechanical model. Restricted or “stiff” joints were thought to require mobilization or manipulation to restore proper alignment and movement. While mechanical factors can play a role, current research suggests that the mechanisms behind manual therapy are more complex.
A combination of mechanical and neurophysiological effects
Some manual techniques can contribute to temporary improvements in joint mobility and tissue flexibility. These changes may help patients move more freely, particularly when pain or stiffness limits daily or sport-specific movements.
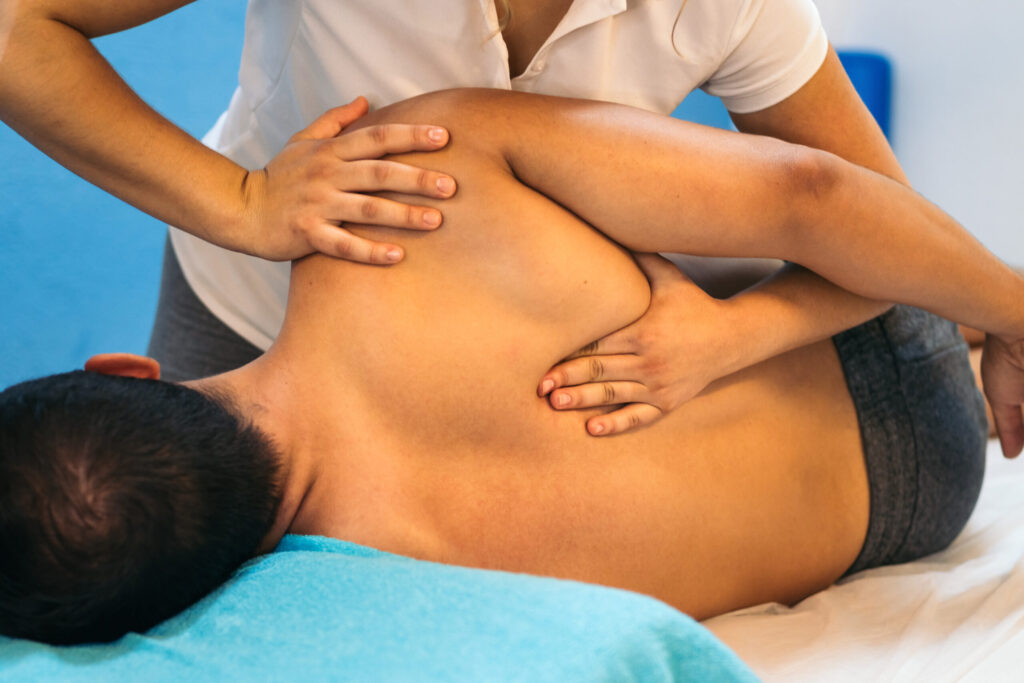
However, the primary effects of manual therapy are now understood to involve the nervous system. Research suggests that hands-on techniques can influence pain modulation, muscle tone and motor control through interactions between peripheral tissues and the central nervous system.
These mechanisms may include:
- modulation of pain perception
- activation of descending inhibitory pathways
- reduction of muscle guarding
- short-term improvements in motor control
- decreased sensitivity to movement
This interaction between the musculoskeletal and nervous systems helps explain why patients often report rapid changes in pain or mobility following treatment.
Short-term improvements that facilitate movement
Manual therapy frequently produces short-term reductions in pain and perceived stiffness. These early changes can be clinically useful, particularly when pain prevents normal movement or participation in rehabilitation.
By decreasing symptoms and improving comfort during movement, manual therapy can help patients:
- move with less apprehension
- regain confidence in movement
- engage more effectively in exercise
- resume daily or sports activities earlier
In this context, manual therapy often acts as a facilitator that prepares patients for more active rehabilitation strategies.
Integrated within a comprehensive rehabilitation approach
In modern physical therapy, manual therapy is rarely used in isolation. It is typically combined with therapeutic exercise, progressive loading and patient education to support long-term recovery.
This integrated approach allows clinicians to use manual therapy to reduce pain and improve movement while simultaneously addressing strength, function and long-term resilience.
3- Is Manual Therapy Effective? What the Evidence Says
Manual therapy is widely used in physical therapy to reduce pain and improve mobility. However, beyond clinical practice, a large body of research has evaluated its effectiveness for various musculoskeletal conditions.
Over the past two decades, systematic reviews and clinical guidelines have provided a clearer understanding of its real impact on pain and function.
Positive effects on pain in the short term
Most studies show that manual therapy can lead to meaningful short-term reductions in pain, particularly in people with low back and neck pain. It can also temporarily improve mobility and reduce the sensation of stiffness.
Research highlights several consistent short-term benefits:
- reduced pain intensity in many musculoskeletal conditions
- temporary improvements in joint mobility
- decreased muscle tension and perceived stiffness
- improved tolerance to movement
A meta-analysis published in The Spine Journal found that manipulation and mobilization techniques can significantly reduce chronic low back pain in the short term (Coulter et al., 2018).
Similarly, a Cochrane review on neck pain reported improvements in pain and function, especially when manual therapy is combined with other interventions such as exercise (Gross et al., Cochrane Review).
These findings suggest that hands-on treatment can be an effective tool to quickly reduce symptoms and help patients re-engage in movement and rehabilitation.
Comparable to exercise for long-term outcomes
When medium- and long-term outcomes are considered, research shows that manual therapy is generally not superior to active interventions such as therapeutic exercise.
Clinical guidelines and large-scale reviews consistently recommend a multimodal approach combining:
- therapeutic exercise
- patient education
- progressive return to activity
- manual therapy when appropriate
The Lancet low back pain series emphasizes that exercise and active rehabilitation strategies are key factors for long-term recovery, while manual therapy should be used as part of a broader management plan (Foster et al., 2018).
Guidelines from the Journal of Orthopaedic & Sports Physical Therapy also support combining physical manipulation with exercise rather than using either approach in isolation (Delitto et al., JOSPT Clinical Practice Guidelines).
Overall, the best outcomes tend to be achieved when manual therapy is integrated with active rehabilitation rather than used as a standalone intervention.
Neurophysiological and contextual effects
Current research suggests that many of the benefits of physical manipulation are linked to neurophysiological mechanisms rather than purely structural changes.
Proposed mechanisms include:
- central modulation of pain
- activation of descending inhibitory pathways
- changes in muscle activation and motor control
- reduced perceived threat associated with movement
These mechanisms, described in models proposed by Bialosky and colleagues (2009), help explain why improvements can occur rapidly even without significant structural changes.
Contextual factors also play a role. The therapeutic alliance, patient expectations and the clinical environment can influence outcomes and contribute to pain modulation and functional improvement (Testa & Rossettini, 2016).
An effective tool, but rarely sufficient alone
Overall, scientific evidence supports a balanced perspective:
- manual therapy can effectively reduce pain in the short term
- it can improve mobility and facilitate movement
- it helps patients engage in rehabilitation
- but it is rarely sufficient on its own for long-term recovery
For sustainable results, manual therapy is most effective when integrated into a comprehensive rehabilitation strategy that includes exercise, progressive loading and patient education.
4- The Role of Manual Therapy in Modern Rehabilitation
Over time, the role of manual therapy in physical therapy has evolved. While it remains a widely used and valuable tool, it is now considered one component of a broader, more comprehensive rehabilitation approach focused on function, activity and long-term outcomes.
Today, the key question is no longer whether manual therapy should be used, but how it can be integrated effectively within modern, evidence-based rehabilitation.
A tool to facilitate movement and reduce pain
Manual therapy can play an important role at the beginning of rehabilitation or during painful phases when movement is limited. By reducing pain and improving perceived mobility, it can help patients move more comfortably and regain confidence.
In clinical practice, manual therapy can:
- reduce pain that limits movement
- temporarily improve joint mobility
- decrease fear or apprehension related to movement
- facilitate participation in exercise
- support early return to activity
Used in this way, manual therapy acts as a facilitator that prepares patients for active rehabilitation rather than replacing it.
A complementary, not standalone, intervention
Modern rehabilitation models emphasize multimodal care. Manual therapy is most effective when combined with active strategies that address strength, function and long-term resilience.
Effective rehabilitation programs often include:
- manual therapy to modulate pain and improve mobility
- therapeutic exercise to restore functio
- progressive strength and conditioning
- motor control and movement retraining
- patient education and self-management strategies
This integrated approach consistently leads to better long-term outcomes than passive treatment alone.
Encouraging an active role for the patient
One of the major goals of contemporary physical therapy is to promote patient autonomy and active participation in recovery. Over-reliance on passive treatments can sometimes reinforce the idea that improvement depends solely on the therapist.
When used appropriately, manual therapy can instead serve as a starting point to:
- reduce symptoms and build trust
- improve tolerance to movement
- restore confidence in physical activity
- encourage engagement in active rehabilitation
This shift from passive care to active participation is central to modern rehabilitation.
Toward more individualized and measurable care
Rehabilitation is increasingly focused on individualized care, functional assessment and measurable outcomes. Within this framework, manual therapy is used strategically to support clearly defined goals.
These goals may include:
- improving mobility
- reducing pain
- restoring strength and function
- supporting return to activity or sport
Combined with regular reassessment and progressive exercise, manual therapy can contribute to meaningful improvements while remaining part of a broader, outcome-driven rehabilitation plan.
5- Conclusion
Manual therapy remains an important component of physical therapy for reducing pain and improving mobility. When used appropriately, it can help patients move more comfortably, regain confidence and prepare for the return to normal activity.
However, current evidence shows that hands-on treatment alone is rarely sufficient to produce lasting outcomes. Long-term recovery is more strongly influenced by active rehabilitation strategies such as therapeutic exercise, progressive loading and patient education.
Modern rehabilitation no longer consists of choosing between manual therapy and exercise, but of integrating them within a comprehensive and individualized treatment approach focused on function and long-term results.
Manual therapy should therefore be viewed not as an end in itself, but as a tool that supports a broader goal: helping patients regain confidence, autonomy and the ability to move sustainably.
6- FAQ: Answer Your Questions about Manual Therapy
What is manual therapy in physical therapy?
Manual therapy refers to a range of hands-on techniques used by physical therapists to reduce pain, improve mobility and restore function. These techniques include joint mobilization, manipulation, soft tissue techniques and neurodynamic interventions.
It is commonly used to manage neuromusculoskeletal conditions such as back and neck pain, joint disorders and sports injuries, and is typically integrated with therapeutic exercise and active rehabilitation.
Is manual therapy evidence-based?
Yes. Research shows that manual therapy can be effective for reducing pain and improving mobility, particularly in the short term. Systematic reviews and clinical guidelines support its use as part of a comprehensive treatment plan.
However, evidence also indicates that manual therapy is most effective when combined with active approaches such as exercise, progressive loading and patient education rather than used alone.
What is the difference between manual therapy and chiropractic care?
Manual therapy is a set of hands-on techniques used within physical therapy to treat musculoskeletal conditions and improve movement. Chiropractic care is a separate healthcare profession that also uses manual techniques, particularly spinal manipulation, but follows a different training pathway and clinical framework.
In physical therapy, manual therapy is usually integrated into a broader rehabilitation program focused on movement, strength and function.
Can manual therapy fix pain permanently?
Manual therapy can help reduce pain and improve mobility, especially in the short term, but it rarely provides a permanent solution on its own. Long-term improvement typically requires active rehabilitation, including exercise, strength training and gradual return to normal activities.
When combined with these approaches, manual therapy can play an important role in supporting sustainable recovery and preventing recurrence.
7- References
- Bialosky, J. E., Bishop, M. D., Price, D. D., Robinson, M. E., & George, S. Z. (2009). The mechanisms of manual therapy in the treatment of musculoskeletal pain: A comprehensive model. Manual Therapy, 14(5), 531–538. https://doi.org/10.1016/j.math.2008.09.001
- Bialosky, J. E., Beneciuk, J. M., & Bishop, M. D. (2018). Manual therapy and pain neuroscience: A proposed model for manual therapy mechanisms. Journal of Orthopaedic & Sports Physical Therapy, 48(1), 8–18. https://doi.org/10.2519/jospt.2018.7476
- Coulter, I. D., Crawford, C., Hurwitz, E. L., Vernon, H., Khorsan, R., Booth, M. S., & Herman, P. M. (2018). Manipulation and mobilization for treating chronic low back pain: A systematic review and meta-analysis. The Spine Journal, 18(5), 866–879. https://doi.org/10.1016/j.spinee.2018.01.013
- Delitto, A., George, S. Z., Van Dillen, L., Whitman, J. M., Sowa, G., Shekelle, P., Denninger, T. R., & Godges, J. J. (2012). Low back pain clinical practice guidelines linked to the International Classification of Functioning, Disability, and Health. Journal of Orthopaedic & Sports Physical Therapy, 42(4), A1–A57. https://doi.org/10.2519/jospt.2012.42.4.A1
- Foster, N. E., Anema, J. R., Cherkin, D., Chou, R., Cohen, S. P., Gross, D. P., Ferreira, P. H., Fritz, J. M., Koes, B. W., Peul, W., Turner, J. A., & Maher, C. G. (2018). Prevention and treatment of low back pain: Evidence, challenges, and promising directions. The Lancet, 391(10137), 2368–2383. https://doi.org/10.1016/S0140-6736(18)30489-6
- Gross, A., Kay, T. M., Paquin, J. P., Blanchette, S., Lalonde, P., Christie, T., Dupont, G., Graham, N., Burnie, S. J., & Goldsmith, C. H. (2015). Manipulation and mobilisation for neck pain contrasted against an inactive control or another active treatment. Cochrane Database of Systematic Reviews, (9). https://doi.org/10.1002/14651858.CD004249.pub4
- Rossettini, G., Carlino, E., & Testa, M. (2020). Clinical relevance of contextual factors as triggers of placebo and nocebo effects in musculoskeletal pain. BMC Musculoskeletal Disorders, 21, 404. https://doi.org/10.1186/s12891-020-03415-1
- Testa, M., & Rossettini, G. (2016). Enhance placebo, avoid nocebo: How contextual factors affect physiotherapy outcomes. Manual Therapy, 24, 65–74. https://doi.org/10.1016/j.math.2016.04.006