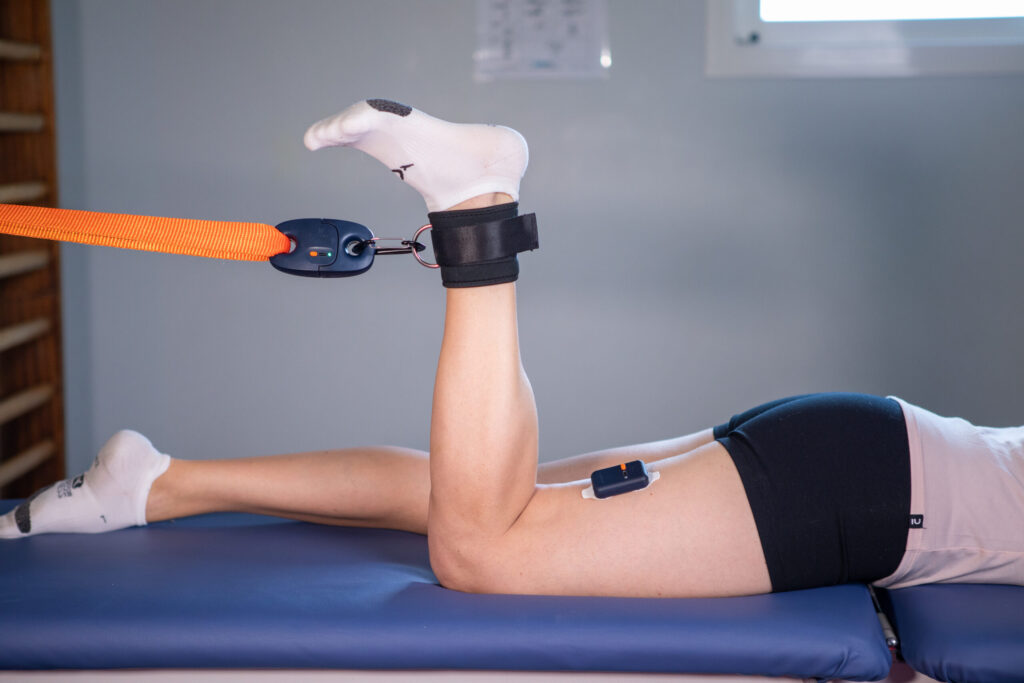
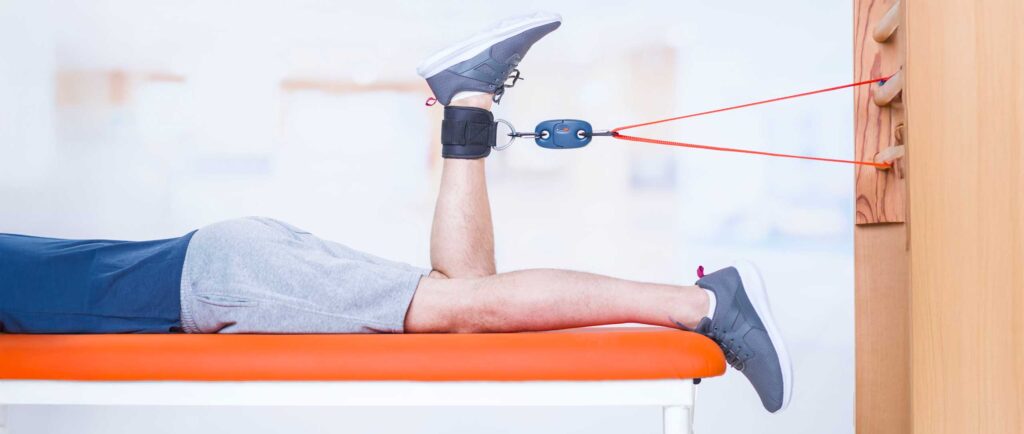
An Anterior Cruciate Ligament (ACL) rupture is one of the most documented sports injuries, yet it remains a major challenge for clinicians. Frequently occurring in pivot, contact, and collision sports (such as soccer, American football, basketball, and skiing), this injury disproportionately affects young and active populations. Recent statistics are striking: the risk of injury is 2.7 to 3.5 times higher for women in these disciplines, with alarming incidence peaks among youth athletes.
Despite increasingly standardized care, the road to full recovery remains fraught with obstacles:
- Only 55% of amateur athletes return to their pre-injury level of competition.
- The recurrence rate can reach 30% among adolescents.
- The risk of a secondary injury is 4 to 7 times higher if a return to sport is premature and not validated by precise criteria.
Given these figures, one truth becomes evident: we do not rehabilitate a pathology; we rehabilitate a patient. The success of the recovery process, whether surgical or conservative, can no longer rely solely on a calendar or a practitioner’s subjective visual assessment.
The future of ACL rehabilitation lies in objective measurement. By integrating connected tools, from surface EMG to 3D force plates, we can now transform every stage of the protocol into a decision based on reliable, reproducible, and safe data.
In this article, we will explore how these technologies optimize every phase of recovery, from overcoming post-operative muscle inhibition to the final return to the field.
CONTENTS
1- What is the ACL?
2- Moving Beyond the Temporal Dogma: You Don’t Rehabilitate a Calendar
3- Phase 1: Muscle Activation and Post-Op (Weeks 0–6)
4- Phase 2: Rehabilitation and Strength Foundations (Months 1–3)
5- Phase 3: Reconditioning, Power, and Plyometrics (Months 3–6)
6- Phase 4: Return to Play (6 – 12 Months)
7- FAQ: Your Questions About ACL Rupture
8- Conclusion
9- References
1- What is the ACL?
The Anterior Cruciate Ligament (ACL) is one of the four primary pillars of knee stability. Located at the core of the joint, it connects the posterior aspect of the femur to the anterior aspect of the tibia.
Its role is fundamental: it acts as a mechanical brake that prevents the tibia from sliding excessively forward (anterior drawer) and controls rotational movements during directional changes
Injury Mechanism and Epidemiology
An ACL rupture typically occurs during indirect trauma without direct contact with an opponent, such as an unbalanced jump landing, a sharp pivot, or sudden deceleration.
Recent scientific data highlight a striking reality in the field:
- High Frequency: It is particularly prevalent in pivot/contact sports like soccer, rugby, handball, or basketball.
- Gender Disparity: Meta-analyses show that the risk is 2.7 to 3.5 times higher in women within these disciplines.
- Variable Incidence: In women’s soccer, there are between 0.09 and 0.32 injuries per 1,000 athletic exposures, compared to 0.02 to 0.12 in men. In professional men’s handball, the global incidence reaches 0.044 per 1,000 exposure hours.
Surgery or Conservative Treatment?
Today, surgical intervention is no longer automatic. Cohort studies, such as the KANON trial, demonstrate that the decision depends on several key factors: activity level (Tegner scale), age, gender, and specifically the presence of associated injuries, such as meniscus or cartilage damage.
For many patients, a well-structured early rehabilitation program can offer clinical results comparable to immediate surgery. Whether surgery is performed or not, the goal remains the same: restoring function to guarantee a safe and high-performance return to play.
2- Moving Beyond the Temporal Dogma: You Don’t Rehabilitate a Calendar
For a long time, ACL rehabilitation was dictated by the passing of months: “return to running at 3 months” or “return to sport at 6 months”. However, time is not an indicator of function. Recent studies show that while ligamentization (the biological healing of the graft) takes time (at least 9 to 12 months), the physical and neuromuscular readiness of a patient varies greatly from one individual to another.
Shifting from Subjective Timeframes to Measurable Objective Criteria
The core challenge lies in returning to performance while minimizing the risk of re-injury. Returning too early without functional validation increases the risk of a new rupture by 4 to 7 times.
Optimizing care now relies on reliable, validated, and reproducible criteria. Instead of asking “What is the date?”, the clinician must ask:
- Is the knee “quiet” (no effusion) and mobile?
- Is the quadriceps lockout (extension) effective?
- Are strength asymmetries between the two legs under control?
The Decisive Role of Connected Tools
This is where technology changes the game. Tools such as EMG sensors, force plates, and portable dynamometers allow us to move from a visual estimation to an indisputable numerical measurement.
These devices, once reserved for elite laboratories, are now accessible in the clinic or directly on the field to guide every stage of progression. They offer immediate feedback, which boosts patient motivation and secures the therapist’s decision-making process.

The Kinvent Solution: We transform your clinic into an analytical laboratory to precisely measure strength, mobility, and motor control at every step of the ACL journey. Thanks to instant biofeedback and progress tracking, you move from subjective feeling to an objective, motivating clinical decision. The entire rehabilitation process is centralized within a single interface.
3- Phase 1: Muscle Activation and Post-Op (Weeks 0–6)
The initial weeks are decisive for the success of the entire protocol. While traditional goals focus on managing pain and edema, as well as regaining range of motion (ROM), two priorities dominate this phase: restoring full extension and overcoming Arthrogenic Muscle Inhibition (AMI).
Overcoming AMI with Surface EMG
Quadriceps inhibition is a post-traumatic reflex mechanism that prevents the muscle from contracting correctly, compromising the knee’s lockout ability. Here, surface EMG (such as the K-Myo) is a game-changer:
- Instant Feedback: Patients see their motor recruitment in real-time on the screen, which facilitates quadriceps stimulation and helps relax the antagonist hamstring muscles.
- Proven Effectiveness: This type of visual feedback significantly accelerates early quadriceps strength recovery.
From Static Balance to Dynamic Control
Before challenging the knee dynamically, it is crucial to objectify postural stability. Force plates are essential here, moving beyond the simple use of a stopwatch:
- Eyes Open (EO) / Eyes Closed (EC) Stabilometry: We precisely measure the surface area of the ellipse of confidence and the velocity of the center of pressure displacement. The goal is to optimize double-leg, then single-leg balance by neutralizing visual compensations before authorizing complex movements.
- Progressive Weight Bearing: Force plates validate weight distribution between the forefoot and hindfoot, as well as right/left symmetry, which is essential for balanced force transmission.
Precise Measurements and Goniometry
When coupled with a connected goniometer (K-Move), these tools allow practitioners to:
- Track ROM recovery to the exact millimeter.
- Use video analysis to identify the slightest compensation during early functional exercises.
- Monitor initial strengthening via a dynamometer to engage the patient through immediate numerical results.
Validation Criteria: To progress to Phase 2, the knee must be quiet (no effusion) and mobile. Active lockout must be achieved (Lag Test ≤ 0 cm), and static postural stability (EO/EC) must be mastered with minimal weight-bearing asymmetry.
4- Phase 2: Rehabilitation and Strength Foundations (Months 1–3)
This phase only begins once the criteria from the previous phase are validated. Weight-bearing asymmetry in a double-leg stance must be minimal before authorizing the transition to full weight-bearing on a single leg.
Securing the Functional Transition
The primary goal is to limit strength asymmetry to safely resume functional exercises such as cycling, stepping, or climbing stairs.
- Validation Criteria (LSI): We aim for a Limb Symmetry Index (LSI) between 20% and 30%, depending on the patient’s activity level, before increasing the load.
- Dynamic Valgus Control: Using video analysis and force plates, we track and correct “medial collapse” (dynamic valgus), particularly during the eccentric phase of lunges or single-leg squats.
- Strengthening the ACL’s “Teammates”: We intensify work on the quadriceps and hamstrings, without forgetting the soleus (a key protector of the graft) and the gluteus medius/adductor pair for frontal stability.
Functional Testing on Force Plates
The use of force plates and manual dynamometers makes the evolution of strength and power quickly quantifiable:
- Posterior Chain and Control: We validate the Single-Leg Hamstring Bridge on a box, the single-leg squat, and lunges to monitor strength gains without compensation.
- Endurance and Propulsion: The Single-Leg Heel Rise Test allows for monitoring the quality of motor control and calf-drive.
- Jump and Landing Analysis: Once control is acquired, we introduce landing tests (e.g., Drop Landing) in a bipodal stance. If force distribution and stability (ellipse of confidence, time to stabilization) are correct, we begin bipodal CMJ (Counter Movement Jump) testing.
- Objectifying Unilateral Motor Control: Functional tests such as the 5 Step Down Test or the Unilateral Sit-to-Stand are essential for evaluating motor control quality. They allow for the precise identification of compensation strategies and validate knee stability before increasing the workload.
The Skipping Test: The Final Gate Before Plicometrics
To prepare for a return to running, we perform an on-the-spot running analysis directly on the force plates (the Skipping Test). This test allows for a precise study of:
- Ground contact time symmetry.
- Forces applied during each strike.
- Flight time (suspension).
Together, these measurements ensure the patient has a solid foundation, validated motor control on one leg, and correct stability to safely engage in intense plyometric challenges.
5- Phase 3: Reconditioning, Power, and Plyometrics (Months 3–6)
This is the phase where everything accelerates and becomes exciting for the patient. While reconditioning can begin early with core or cardio exercises, it truly takes off with the resumption of running and multi-directional loading. We move beyond “classical” rehab to intensely develop the patient’s athletic and neurocognitive capacities.
The Neurocognitive Shift: Preparing the Brain for the Field
In this phase, neurocognitive training, specifically dual-tasking, becomes a priority. The goal is to challenge memory, focus, and reactivity to promote the neural plasticity essential for motor control in a game situation.
- Connected Tools: Using reaction lights (Neural Trainer, BlazePods, Sportreact, etc.) allows for combining colors, numbers, and shapes to precisely measure reaction times.
- Vision and Coordination: Devices like NeuroTracker or simpler tools like “Catch and Think” help perfect the patient’s complete “grounding” and spatial awareness.
Jump Continuum and Unilateral Plyometrics
We revisit the entire exercise battery in a single-leg format and through jump sequences (plyometrics), exploring all three planes of motion.
- Symmetry Requirements: Tolerance for strength asymmetries (Quadriceps/Hamstrings) tightens, with a target deficit of less than 20%.
- Test Batteries: We utilize the Hop Tests (Single, Triple, Crossover, Side Hop), the full range of functional tests as seen in the K-STARTS protocol, and psychological assessments like the ACL-RSI.
- Precision of Force Plates: Force plates replace the stopwatch or measuring tape by providing data on power, velocity, and the RSI (Reactive Strength Index) during a Drop Jump.
The “Game Changers”: 3D Analysis and VBT
To detect deficits invisible to the naked eye, two tools become decisive:
- 3D Force Plates (3D Deltas): These allow for the exploration of lateral and anteroposterior planes. Analyzing Force/Time curves during a change of direction or a Skater Jump reveals avoidance strategies that are undetectable in the vertical plane alone.

💡 Want to learn more? Check out our article on 3D motion analysis.
2. Velocity-Based Training (VBT): Using the velocity sensor (K-Power), we move away from theoretical 1RM calculations to monitoring based on execution speed. This ensures work stays within the correct physiological zone (explosiveness) while precisely monitoring fatigue.
Horizontal Velocity and Force-Velocity Profiling

The K-Power hybrid sensor also enables horizontal velocity analysis via 10-to-50-meter sprints. Without time-consuming setups, you instantly obtain:
- Max velocity, power, and the Force-Velocity profile.
- Precise analysis of a Triple Hop Test or a shuttle run (Agility T-test), with higher objectivity than a manual stopwatch.
By following a strict progression logic (landing, then jumping, then Drop Jumps and multi-planar exits), these precise measurements (CMJ, Skater Jump, Max Strength) become real performance indicators shareable with the physician, surgeon, coach, or athletic trainer.
6- Phase 4: Return to Play (6–12 Months)
This final stage aims to ensure the patient can return to their previous activities and competition with maximum safety. While timeframes (6, 9, or 12 months) are often used as benchmarks, they are insufficient on their own to validate a risk-free return to the field.
Objective Evaluation: Recovering the Athlete
It is precisely in this phase that we look to restore the full spectrum of athletic qualities: stability, power, endurance, explosiveness, and speed.
- Performance Standards: We aim to match or exceed pre-season standards or the patient’s historical “baseline” data across all energy systems. It is the moment to revisit the entire battery of functional tests performed in previous phases, ensuring they are now comparable to the healthy limb and to the athlete’s pre-injury performance (YBT, Triple Hop, Hop Test, Broad Jump, Test de navette, Drop Jump, Skater Jump, etc.).
- Force-Velocity Profiling: Utilizing horizontal profiles (sprints) and vertical profiles (Squat Jumps) helps optimize the final gains needed in strength or explosiveness.
- Advanced Indices: We rely on quality ratios like the RSI (Reactive Strength Index) or the DSI (Dynamic Strength Index) to validate braking and propulsion capabilities.
- Symmetry Requirements: Tolerance for right/left asymmetries sharpens, with a target deficit of less than 10% (or 15% for recreational athletes).
Centralization: From Evaluation to Training
The major advantage of the Kinvent ecosystem lies in the total centralization of care within a single application.
- Training Modes and feedback: You can instantly switch from testing to specific training modes like “Tempo Training.” This mode allows you to parameterize every phase of a movement (concentric, isometric, eccentric) for ultra-high-quality work.
- Motor Learning: With real-time visual feedback on the screen, the patient adjusts their force or positioning instantly. This immediate biofeedback facilitates the removal of inhibitions and allows the patient to track their own progress.
- Clinical Efficiency: Everything is recorded in one place, allowing you to visualize the progress curve in one click and schedule sessions via the integrated MyKinvent calendar.
The Human Element: Managing Apprehension
While data is essential, it must not overshadow the patient’s subjective experience. Field tests, technical drills, and the gradual return to contact are stages where the road can still feel long.
- Fear of Re-injury: The psychological aspect is a pillar of success. Persistent apprehension can alter movement biomechanics and increase the risk of recurrence, even if athletic capacities seem restored.
- Validated questionnaires, such as the ACL-RSI, measure the athlete’s confidence level and detect any underlying fear of re-injury.
- This final phase is the ultimate example of close collaboration between the physician, physical therapist, strength & conditioning coach, sport coach and patient.
Confronting reliable data and technological “green lights” with the athlete’s deep-seated feelings allows for refined return criteria. This holistic approach strengthens the essential bond of trust between the therapist and the patient, from the treatment table back to the field.
7- FAQ: Your Questions About ACL Rupture
Is surgery mandatory?
No, surgery is no longer systematic. The decision depends on your activity level (Tegner scale), age, gender, and the presence of associated injuries (meniscus, cartilage). Recent studies, such as the KANON trial, show that a well-structured early rehabilitation program can offer clinical results comparable to immediate surgery for many patients.
What is the success rate of ACL reconstruction?
While 85% to 92% of professional athletes return to their competitive level, this figure drops to only 55% among recreational athletes across all levels. This gap highlights the importance of management based on objective criteria rather than just timeframes to guarantee a safe return to performance.
Why is the risk of re-injury so high?
The recurrence rate is significant: it ranges between 15% and 23% in young athletes and can reach 30% in adolescents. Returning to sport too early, without validating strength criteria (LSI) and motor control, multiplies this risk by 4 to 7. The use of connected tools helps detect “invisible” deficits that are often the root cause of these secondary injuries.
When can I start running again?
Resuming running (usually around month 3) is only authorized if several “green lights” are met:
- A “quiet” knee (no effusion), mobile and reactive.
- Acquired and objectified active extension (Lag Test).
- Strength asymmetry (LSI) of less than 30% between the two legs.
- Validated single-leg motor control, with corrected dynamic valgus, especially during the eccentric phase, and high-quality landing and shock absorption mechanics.
- Correct stability confirmed by on-the-spot running tests (Skipping Test) on force plates.
8- Conclusion
The care pathway following an ACL injury is a demanding journey, paced by incompressible biological and mechanical stages. While manual therapy remains a pillar of management, the contribution of connected tools marks a major turning point in our practice.
By moving from the subjective to the objective, we remove the uncertainties that traditionally surround the return to sport. These technologies do not replace the clinician’s expertise; they augment it by offering:
- Instant Feedback: Strengthening patient engagement and motivation.
- Rigorous Traceability: Allowing for the visualization of 6 to 12 months of progress in a single click.
- Increased Safety: Basing every phase transition on validated performance criteria rather than simple temporal delays.
The final goal remains the same: a serene, high-performance return to the field, and above all, without apprehension.
9- References
- Frobell RB, et al. A randomized trial of treatment for acute anterior cruciate ligament tears. N Engl J Med. 2010;363(4):331-42.
- Lohmander LS, et al. Treatment for acute anterior cruciate ligament tear: 11-year follow-up. NEJM Evidence. 2023;2(2).
- Ardern CL, et al. Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: an updated systematic review and meta-analysis. Br J Sports Med. 2014;48(21):1543-52.
- D’Ambrosi R, et al. The majority of elite and professional athletes return to the preinjury level of activity after ACL reconstruction: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2025 (online).
- D’Ambrosi R, et al. Slower but not safer: a systematic review and meta-analysis of return to play and graft re-rupture after ACL reconstruction in professional soccer players. Sports Med Open. 2025;11(1):157.
- Montalvo AM, et al. Anterior cruciate ligament injury risk in sport: a systematic review and meta-analysis of injury incidence by sex and sport classification. J Athl Train. 2019;54(5):472-82.
- Prodromos CC, et al. A meta-analysis of the incidence of anterior cruciate ligament tears as a function of gender, sport, and a knee injury-reduction regimen. Arthroscopy. 2007;23(12):1320-5.
- Martinez-Calderon J, et al. The incidence of sport-related anterior cruciate ligament injuries: an overview of systematic reviews including 51 meta-analyses. J Funct Morphol Kinesiol. 2025;10(2):174.
- Wiggins AJ, et al. Risk of secondary injury in younger athletes after ACL reconstruction. Am J Sports Med. 2016;44(8):1861-76.
- Barber-Westin SD, et al. One in 5 athletes sustain reinjury upon return to high-risk sports after ACL reconstruction. Orthop J Sports Med. 2020;8(12):2325967120969375.
- Moiroux-Sahraoui A, et al. Quadriceps activation after anterior cruciate ligament reconstruction: the early bird gets the worm! Int J Sports Phys Ther. 2024;19(4):468-78.
- Ananías J, et al. Use of electromyographic biofeedback in rehabilitation following ACL reconstruction: systematic review and meta-analysis. Physiotherapy. 2024;123:1-10.
- Blakeney WG, et al. Validation of the K-STARTS test. Am J Sports Med. 2018;46(9):2118-25.
- Gerfroit A, et al. Establishing threshold values for the patient acceptable symptom state after anterior cruciate ligament reconstruction: the SKV and ACL-RSI scales. Orthop J Sports Med. 2025 (in press).
- Forelli F, et al. Velocity-based training in mid- and late-stage rehabilitation after ACLR. BMJ Open Sport Exerc Med. 2025;11(2):e002503.
- Filbay SR, et al. Evidence of ACL healing on MRI following ACL rupture treated with rehabilitation alone may be associated with better patient-reported outcomes: a secondary analysis from the KANON trial. Br J Sports Med. 2023;57(2):91-8.
- Kotsifaki R, et al. Single-leg vertical jump performance identifies knee function deficits at return to sport after ACL reconstruction in male athletes. Br J Sports Med. 2022;56(9):490-6.
- Chia L, et al. Non-contact anterior cruciate ligament injury epidemiology in team-ball sports: a systematic review with meta-analysis by sex, age, sport, participation level, and exposure type. Sports Med. 2022;52(10):2447-62.