Low back pain is one of the most common issues in adults. It can show up suddenly after an effort or build up over time, making work, sports, and everyday movements harder. The pain can feel alarming, but in most cases it’s linked to a functional problem rather than a serious injury.
Scientific understanding of low back pain has evolved significantly in recent years. Current recommendations emphasize that the back primarily needs movement, properly functioning muscles, and improved motor control to recover. Prolonged rest or avoiding activity out of fear of pain can actually slow down recovery instead of helping.
This article draws on findings from recent research to present a clear, evidence-based practice (EBP) approach. The goal is to better understand low back pain and provide practical, progressive, and individualized guidance.
In this article, we’ll explain what low back pain is, the most common causes, when you should seek medical advice quickly, and what you can do to relieve symptoms. We’ll also cover the role of exercise, movement, and functional assessment to reduce recurrence and help you build a stronger, more confident back over time.
CONTENTS
1- What is Low Back Pain?
2- Why Does Your Lower Back Hurt? Understanding the Mechanism
3- When Should You Worry About Low Back Pain?
4- Low Back Pain Assessment Protocol: A Structured, Evidence-Based Approach
5- Low Back Pain and Sports: How to Prevent Recurrence
6- Key Takeaways
7- Frequently Asked Questions (FAQ)
8- References
1- What is Low Back Pain?
Low back pain is often called “the disease of the century.” In reality, it’s more accurately the problem of sedentary living and poorly managed movement. Low back pain isn’t a disease; it’s a symptom, and it’s now one of the leading causes of disability worldwide.
A very common condition
A few numbers help illustrate the scope of the issue:
- At any given time, 12–33% of adults report low back pain (Hartvigsen et al., 2018)
- About 8 out of 10 people will experience low back pain at least once in their lifetime
- After a first episode, the risk of recurrence within a year is high
Low back pain also has a major impact at work:
- It’s one of the leading causes of work absence before age 45
- Only a small percentage becomes chronic, but persistent cases account for most costs and day-to-day limitations
The “sports paradox”
You’ll often hear that exercise protects your back. That’s true, as long as the load is appropriate.
- Too little physical activity can weaken the system
- But very intense or poorly balanced training can also increase risk

Some sports place higher stress on the lower back, such as:
- Gymnastics, with repeated hyperextension and high impacts
- Rowing, with repeated loaded flexion
- Golf and tennis, with repetitive asymmetrical rotation
So athletes aren’t immune: the back can suffer from too little movement and from high loads that aren’t well managed.
2- Why Does Your Lower Back Hurt? Understanding the Mechanism
To understand low back pain, it helps to see the back as a system that needs balance. Spinal stability relies on three components working together (Panjabi, 1992):
- Passive system (structures): vertebrae, discs, ligaments
- Active system (muscles): support and protect the spine
- Neural system (motor control): coordination between the brain and muscles
Pain often appears when muscle function and motor control can’t compensate well enough for external stress and internal demands. That’s why low back pain is rarely “just a disc” or “just a bone”; it’s often a global function issue.
We don’t focus only on pain anymore
Modern low back pain management isn’t just about rating pain intensity. What matters most is your ability to move and function day to day.
Recent research shows that:
- simple physical tests can help predict return to work and return to sport
- imaging (X-ray, MRI) often doesn’t explain pain intensity or real-life function
- about 85% of low back pain is non-specific, with no serious injury identified
- many patients show delayed muscle activation and altered movement control
👉 That’s why assessing how the back moves and how muscles do their job matters just as much as symptoms.
The low back pain vicious cycle
Low back pain can easily create a cycle that’s hard to break:
- pain leads to fear of movement
- activity decreases
- muscles weaken and the body stiffens
- the back becomes more sensitive… and pain returns
That’s why the key message is clear: prolonged strict rest is rarely the solution. In most cases, the main treatment is progressive, adapted movement.
The low back: a “crossroads” area
The lumbar spine is a hinge between the upper and lower body. When areas around it don’t move well, the low back often compensates.
- Limited hip or ankle mobility can overload the low back
- A stiff thoracic spine can force the lumbar spine to rotate too much
- Repeated compensations can maintain symptoms
In other words, lasting relief usually requires looking beyond the painful area and considering the whole body in motion.
3- When Should You Worry About Low Back Pain?
Most cases are benign mechanical pain related to how muscles and joints are functioning. Pain can be intense and frightening, but it’s most often not linked to a serious injury.
That said, certain situations require quick medical advice. These warning signs are uncommon, but important.
Red flags: when to seek medical care quickly
See a doctor promptly if low back pain comes with:
- fever, chills, or feeling generally unwell
- unexplained weight loss
- pain after major trauma (fall, car accident)
- worsening weakness in one leg
- unusual bladder or bowel issues (difficulty urinating, loss of control)
- loss of sensation in the groin/perineal area
These symptoms can suggest a more serious condition and should be assessed quickly.
In most cases, low back pain is not serious
When red flags are not present:
- pain is most often non-specific
- imaging is not always needed at the beginning
- the back remains strong, even when painful
Pain often reflects a mix of factors: limited mobility, fatigued muscles, repetitive loads, stress, or poor sleep. It can hurt a lot without meaning the back is “damaged forever.”
The best reflex: stay as active as possible
Unless a healthcare professional tells you otherwise:
- keep moving within tolerable limits
- avoiding movement completely can maintain pain
- gradually resuming daily activities supports recovery
💡Key message: adapted movement is part of the treatment.
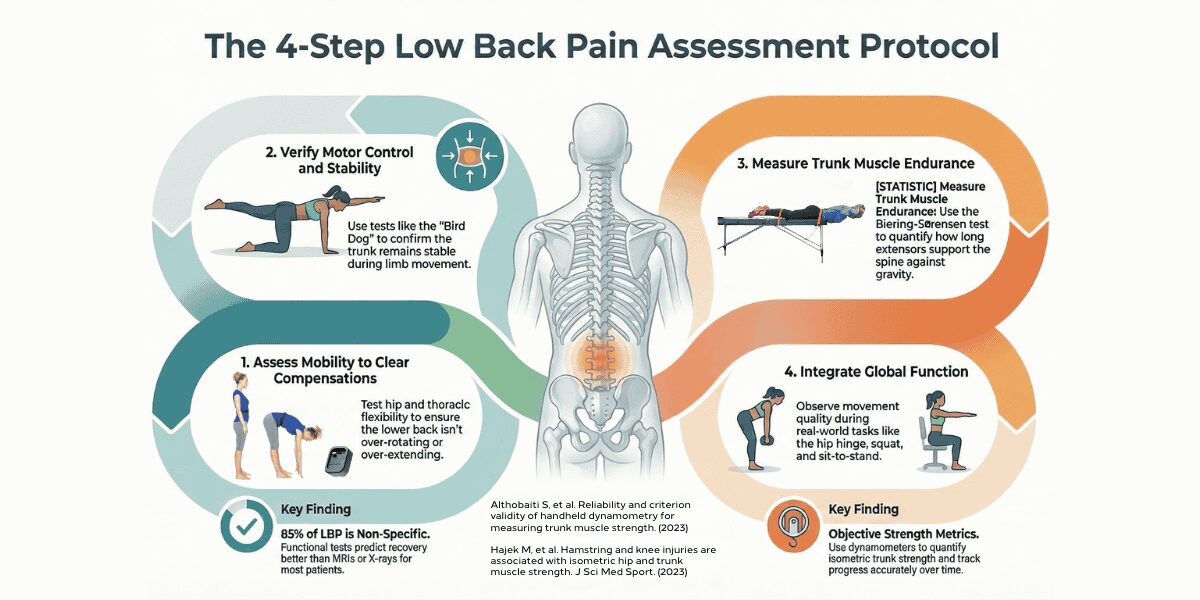
4- Low Back Pain Assessment Protocol: A Structured, Evidence-Based Approach
For physical therapists, modern low back pain care relies on progressive, functional assessment. The goal isn’t only to measure pain, but to understand how the body moves, stabilizes, and handles load.
This approach follows a science-backed sequence used in rehab and performance: mobility → motor control → endurance → function
Step 1: Assess mobility
First, check if certain areas lack range of motion, which may force the lower back to compensate.
- Finger-to-floor test
→ Measures forward bending ability and gives a global view of posterior chain flexibility.

- Modified Thomas test
→ Assesses hip flexor flexibility; stiffness here may increase lumbar extension. - Supine hip rotation assessment
→ Identifies left/right hip rotation differences often linked to lumbar compensations. - Thoracic rotation tests (Open Book, seated rotation)
→ Measures upper-back rotation capacity to prevent excessive lumbar rotation. - Leg Lateral Reach Test (LLRT)
→ A functional test observing the combined mobility of pelvis, trunk, and hips during a lateral reach pattern.
Step 2: Assess motor control and stability
Mobility alone isn’t enough; you also need control.
- Waiter’s Bow (controlled hip hinge)
→ Observes the ability to hinge at the hips without excessive lumbar rounding. - Standing pelvic control (anterior/posterior tilt)
→ Assesses pelvic dissociation and lumbopelvic control. - Bird Dog
→ Contralateral arm/leg coordination test showing trunk stability during limb movement. - Swiss ball stability (seated or kneeling balance)
→ Highlights trunk control in mildly unstable conditions.
Step 3: Measure trunk muscle endurance
The back muscles must have good endurance capacity.
- Biering-Sørensen test
→ Measures how long the spinal extensor muscles can maintain the trunk in a horizontal position against gravity.

- Shirado-Ito test
→ Assesses abdominal endurance in a sustained semi-sit position. A hold time of more than 2 minutes is a good indicator. Below 1 minute, the risk of developing low back pain is significant.

- Flexor/extensor endurance ratios
→ Compares the endurance of the anterior and posterior trunk muscles to identify potential imbalances.
- Single Leg Hamstring Bridge
→ Posterior chain endurance test (hamstrings and glutes), working in synergy with the low back.
💡 Additional: objective measures of trunk strength and mobility
For some patients or athletes, assessment can be refined using objective measures of isometric trunk strength and trunk range of motion. These metrics help quantify deficits and track progress more precisely over time.
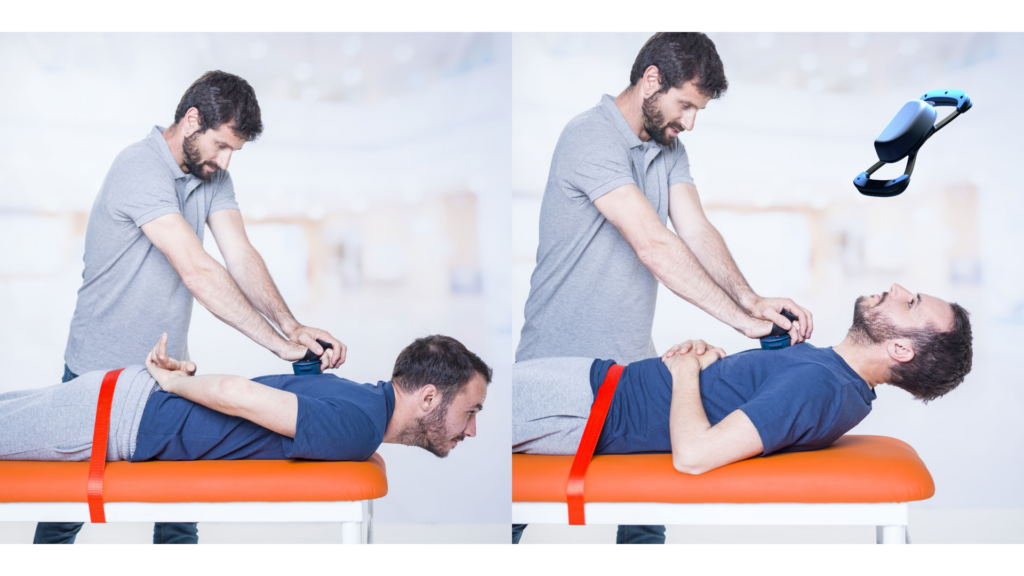
- Isometric lumbar extension (instrumented Sorensen-style position)
→ Quantifies back extensor force in a static position, detecting strength deficits or asymmetry. - Standing isometric trunk flexor and extensor testing
→ Provides a reproducible way to analyze the balance between anterior and posterior trunk muscles, which supports lumbar stability. - Goniometric range-of-motion measures
→ Assessment of trunk flexion, extension, rotation, and side-bending range of motion helps identify mobility restrictions that may lead to lumbar compensations.
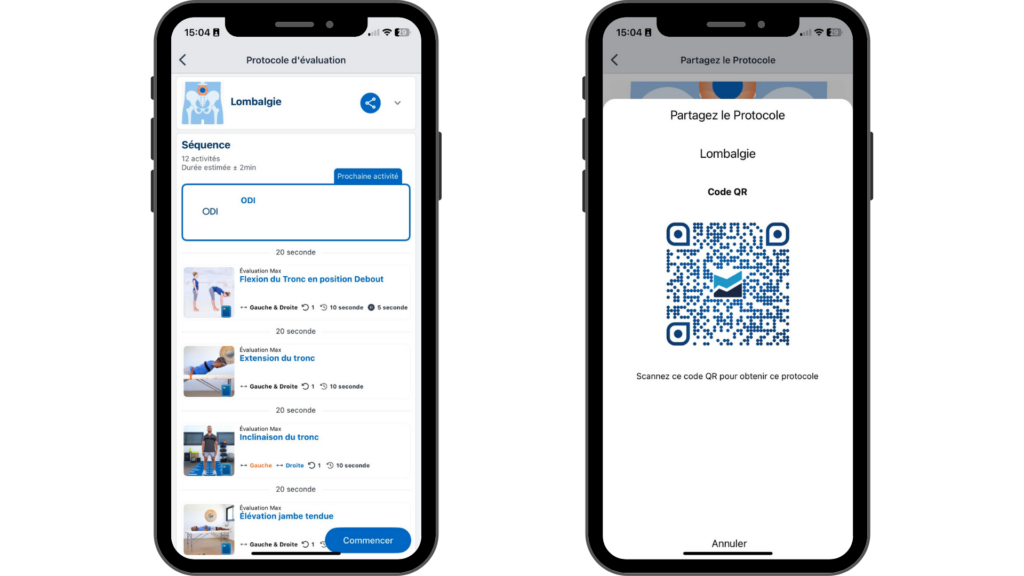
In this context, Kinvent tools such as K-Push (handheld dynamometer) and K-Move (goniometer) allow clinicians to capture standardized, reliable measurements. The data integrates directly into the Kinvent app, which includes a dedicated Low Back Pain protocol to guide clinicians through mobility testing, isometric strength measures, and session-to-session progress tracking.
Step 4: Integrate the global function
Finally, observe the body in movements closer to real life.
- Hip hinge
→ Assesses bending mechanics using the hips rather than lumbar compensation. - Squat
→ Observes coordination across hips, knees, and trunk during a global movement. - Back Performance Scale (BPS) functional tests
→ A series of simple tasks (sit-to-stand, bending, turning) assessing how low back pain affects everyday activities.
Evidence-informed and tailored
Recent studies suggest that:
- functional tests can predict return to work better than imaging alone
- ~85% of cases are non-specific with no serious structural cause
- low back pain patients often show deficits in motor control and muscle endurance
This protocol helps target real overload factors rather than focusing only on anatomical structure.
5- Low Back Pain and Sports: How to Prevent Recurrence
Having low back pain doesn’t mean you must stop training forever. A progressive, well-guided return is part of recovery. The key is to follow steps that reduce relapse risk.
The goal isn’t just to reduce pain, but to prepare the back to tolerate movement and training demands again.
Step 1: Return to movement with manageable symptoms
Before returning to training:
- daily movements (walking, bending, standing up) should feel easier
- hip and thoracic mobility should improve
- trunk control exercises should be performed without major compensation
Step 2: Restore trunk endurance
Sports involve repeated load, so the back needs stamina.
Before higher intensity returns, it’s useful to:
- improve the endurance of the paraspinal muscles
- train deep core control and pelvic stability
- include glutes and hamstrings to unload the lumbar spine
Step 3: Reintroduce sport-specific demands
Each sport stresses the back differently:
- rotation in tennis and golf
- repeated flexion in rowing
- impacts and hyperextension in gymnastics
- contact and cutting in team sports
Return should progressively include:
- movements close to the sport pattern
- gradual increases in load and intensity
- focus on movement quality
Step 4: Monitor symptoms
Mild discomfort may be normal. But slow down if you notice:
- clear pain increases after training
- marked next-day stiffness that doesn’t improve
- feeling unstable or losing control
In those cases, adjust the load rather than stopping completely.
Key principle: progress without rushing
Return to sport after low back pain should be:
- progressive
- tailored to the individual and the sport
- focused on movement quality more than immediate performance
Done well, training becomes an ally: it strengthens the back, builds confidence, and reduces recurrence risk.
6- Key Takeaways
Low back pain is very common and can be alarming… but it is most often related to how the body is functioning rather than to a serious injury. Understanding this can reduce worry and help you act.
Key points to remember:
- Low back pain is a symptom, not a disease
- In most cases, it’s non-specific and linked to movement, muscle function, and lifestyle
- Prolonged strict rest usually isn’t the answer; adapted movement supports recovery
- The low back doesn’t work alone: hip and thoracic mobility matter
- Trunk muscles should be endurance-focused, not only “strong”
- Effective care follows a sequence: mobility → motor control → endurance → gradual return to activity
- Regaining confidence in movement helps prevent the pain–fear–avoidance cycle
Prevention is simple but consistent: move often, maintain mobility, and keep muscles active. The back is built for movement, well supported and progressively trained; it can become a reliable ally again.
7- Frequently Asked Questions (FAQ)
How long does low back pain last?
Acute low back pain usually lasts from a few days to a few weeks, often improving gradually. Chronic low back pain is defined as pain lasting longer than 3 months. In that case, factors like reduced movement and fear of pain may contribute to persistence.
Should you stop moving when your back hurts?
Usually no. Prolonged strict rest can slow recovery. Staying active within tolerable limits and gradually resuming daily activities helps the back regain function.
What are the best exercises for low back pain?
The most effective work typically targets:
- hip and thoracic mobility
- trunk control
- endurance of the back extensors and deep core muscles
A progressive, individualized program works better than random exercises.
Can you play sports with low back pain?
Yes, in most cases. You can often continue or return progressively by adjusting intensity, restoring mobility and trunk endurance, then rebuilding sport-specific demands step by step. A sudden return increases recurrence risk.
Why does low back pain come back so often?
Recurrence happens because:
- root causes (stiffness, weakness, poor control) aren’t addressed
- activity returns too fast or stops for too long
- fear of movement leads to avoidance and deconditioning
Prevention relies on regular activity plus maintaining mobility and trunk endurance.
8- References
- Adedoyin RA, et al. Endurance of low back musculature: Normative data for adults. J Back Musculoskelet Rehabil. 2011;24(3):119-127. DOI: 10.3233/BMR-2011-0288.
- Althobaiti S, et al. Reliability and criterion validity of handheld dynamometry for measuring trunk muscle strength. Musculoskelet Sci Pract. 2023;62:102612. DOI: 10.1016/j.msksp.2022.102612.
- Askling C, et al. Hamstring injury prevention in elite football: The Nordic Hamstring Exercise revisited. Br J Sports Med. 2021;55(1):1-2. DOI: 10.1136/bjsports-2020-103520.
- Berglund L, et al. Which Patients With Low Back Pain Benefit From Deadlift Training? J Strength Cond Res. 2015;29(7):1935-1940. DOI: 10.1519/JSC.0000000000000827.
- Biering-Sørensen F. Physical measurements as risk indicators for low-back trouble over a one-year period. Spine. 1984;9(2):106-119. DOI: 10.1097/00007632-198403000-00002.
- Chou R, et al. Imaging strategies for low-back pain: systematic review and meta-analysis. Lancet. 2009;373(9662):463-472. DOI: 10.1016/S0140-6736(09)60172-0.
- Demoulin C, et al. Spinal muscle evaluation using the Sorensen test: a critical appraisal of the literature. Joint Bone Spine. 2006;73(1):43-50. DOI: 10.1016/j.jbspin.2004.11.010.
- Ekedahl H, et al. Validity of the Fingertip-to-floor test and Straight leg raising test. Arch Phys Med Rehabil. 2010;91(9):1437-1443. DOI: 10.1016/j.apmr.2010.06.016.
- Fairbank JC, et al. The Oswestry low back pain disability questionnaire. Physiotherapy. 1980;66(8):271-273. PMID: 6452736. https://pubmed.ncbi.nlm.nih.gov/6450426/
- Freckleton G, et al. The predictive validity of a single leg bridge test for hamstring injuries. Br J Sports Med. 2014;48(8):713-717. DOI: 10.1136/bjsports-2013-092262.
- Haischer MH, et al. Impulse-Based Dynamic Strength Index: Considering Time-Dependent Force Expression. J Strength Cond Res. 2021;35(4):927-933. DOI: 10.1519/JSC.0000000000003942.
- Hajek M, et al. Hamstring and knee injuries are associated with isometric hip and trunk muscle strength. J Sci Med Sport. 2023;26(3):245-250. DOI: 10.1016/j.jsams.2022.11.005.
- Hartvigsen J, et al. What low back pain is and why we need to pay attention. Lancet. 2018;391(10137):2356-2367. DOI: 10.1016/S0140-6736(18)30480-X.
- HAS. Prise en charge du patient présentant une lombalgie commune. Recommandations de bonne pratique. 2019.
- Hodges PW, Richardson CA. Inefficient muscular stabilization of the lumbar spine associated with low back pain. Spine. 1996;21(22):2640-2650. DOI: 10.1097/00007632-199611150-00014.
- Hoy D, et al. The global burden of low back pain. Ann Rheum Dis. 2012;71(6):979-985. DOI: 10.1136/annrheumdis-2011-200344.
- Hurri H, et al. Functional Tests Predicting Return to Work. Int J Environ Res Public Health. 2023;20(5):4231. DOI: 10.3390/ijerph20054231.
- Ito T, et al. Lumbar trunk muscle endurance testing. Arch Phys Med Rehabil. 1996;77(4):414-417. DOI: 10.1016/S0003-9993(96)90132-0.
- Johnson KD, et al. Thoracic rotation measurement reliability. J Orthop Sports Phys Ther. 2012;42(7):A1-A48. DOI: 10.2519/jospt.2012.42.7.A1.
- Katz K, et al. Normal ranges of popliteal angle in children. J Pediatr Orthop. 1992;12(2):229-231. DOI: 10.1097/01241398-199203000-00015.
- Kendall FP, et al. Muscles: Testing and Function, with Posture and Pain. 5th ed. Lippincott Williams & Wilkins; 2005.
- Kim S-H, et al. Leg lateral reach test reliability. J Sci Med Sport. 2016;19(10):795-799. DOI: 10.1016/j.jsams.2015.10.004.
- Kopec JA, et al. The Quebec Back Pain Disability Scale. Spine. 1995;20(3):341-352. DOI: 10.1097/00007632-199502000-00014.
- López-Miñarro PA, et al. Sit-and-reach vs back-saver sit-and-reach. J Sports Sci Med. 2009;8(2):203-208.
- Luomajoki H, et al. Movement control tests of the low back. BMC Musculoskelet Disord. 2008;9:170. DOI: 10.1186/1471-2474-9-170.
- McGill SM. Low Back Disorders: Evidence-Based Prevention and Rehabilitation. Human Kinetics; 2007.
- Moreau CE, et al. Fatigue in trunk extensors during sustained isometric contractions. Eur J Appl Physiol. 2015;115(6):1261-1270. DOI: 10.1007/s00421-015-3125-8.
- Oliva-Lozano JM, et al. Protocoles personnalisés pour LBP en haltérophilie et gymnastique. J Strength Cond Res. 2023;37(4):789-796. DOI: 10.1519/JSC.0000000000004321.
- OMS (WHO). Guidelines on physical activity and sedentary behaviour. 2020.
- Panjabi MM. The stabilizing system of the spine. J Spinal Disord. 1992;5(4):383-389.
- Perret C, et al. Flexibility of the back and hamstrings in low back pain patients. Eur J Phys Med Rehabil. 2001;11(3):119-123.
- Pfingsten M, et al. Significance of physical performance tests for patients with low back pain. Pain Med. 2014;15(2):289-297. DOI: 10.1111/pme.12279.
- Reyes-Ferrada W, et al. Muscle Quality and Functional Ratios of Trunk Strength. Int J Environ Res Public Health. 2022;19(3):1456. DOI: 10.3390/ijerph19031456.
- Reyes-Ferrada W, et al. Reliability of trunk strength measurements with an isokinetic dynamometer. J Back Musculoskelet Rehabil. 2022;35(4):865-874. DOI: 10.3233/BMR-210289.
- Richardson CA, et al. Therapeutic exercise for lumbopelvic stabilization. Churchill Livingstone; 1998.
- Resende RA, et al. Does trunk and hip muscles strength predict performance during a core stability test? Braz J Phys Ther. 2019;23(3):235-241. DOI: 10.1016/j.bjpt.2018.09.003.
- Shirado O, et al. Quantitative assessment of abdominal muscular function. Arch Phys Med Rehabil. 1995;76(1):14-18. DOI: 10.1016/S0003-9993(95)80025-3.
- Stanton R, et al. Sensory system manipulation and balance control. J Mot Behav. 2011;43(1):17-23. DOI: 10.1080/00222895.2010.535127.
- Strand LI, et al. Back Performance Scale. Phys Ther. 2002;82(12):1213-1223. DOI: 10.1093/ptj/82.12.1213.
- Tidstrand J, Horneij E. Inter-rater reliability of functional tests in low back pain. BMC Musculoskelet Disord. 2009;10:59. DOI: 10.1186/1471-2474-10-59.
- Van Dillen LR, et al. Movement system impairment-based classification. Phys Ther. 2008;88(9):1071-1082. DOI: 10.2522/ptj.20070289.
- Waddell G, et al. Fear-avoidance beliefs questionnaire (FABQ). Pain. 1993;52(2):157-168. DOI: 10.1016/0304-3959(93)90113-B.
- Welch N, et al. Effects of free weight deadlifts on chronic low back pain. J Strength Cond Res. 2015;29(7):1935-1940. DOI: 10.1519/JSC.0000000000000827.
- Zemková E, et al. Peak Rate of Force Development and Isometric Maximum Strength of Back Muscles. Am J Mens Health. 2019;13(4):1557988319862196. DOI: 10.1177/1557988319862196.
- Zerkak D, et al. Validation of a French version of Roland-Morris questionnaire. Ann Phys Rehabil Med. 2013;56(4):257-269. DOI: 10.1016/j.rehab.2013.02.006.