Ankle sprains are the most common injury in the sporting world, representing approximately 25% of sports injuries across all disciplines (Doherty C et al. 2014). However, behind this apparent banality lies a major public health issue: 40% to 70% of patients develop Chronic Ankle Instability (CAI) after an initial episode that was poorly managed.
Today, evolving clinical practices demand a shift from rehabilitation based on simple “time-to-rest” to an approach guided by objective and measurable criteria.
In this article, we detail:
- Injury mechanisms and the risks of chronicity.
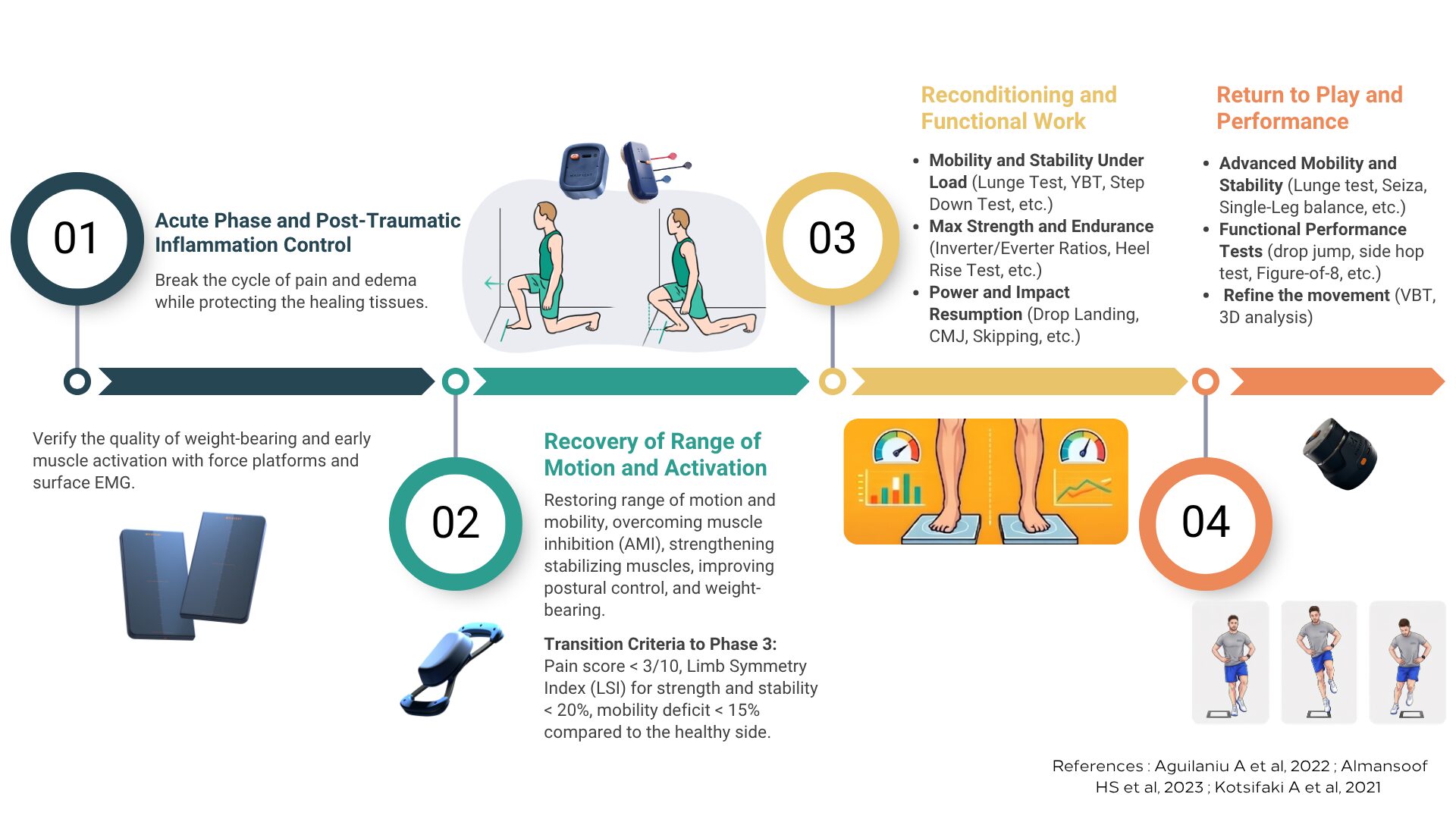
- A rehabilitation protocol is divided into four key phases: Acute, Subacute, Reconditioning (Return to Play), and Return to Competition.
- The contribution of Kinvent’s connected tools to the objective measurement of strength, range of motion, and sensorimotor control.
- Synergy with TECAR therapy to remove mobility restrictions and accelerate drainage.
CONTENTS
1- What is an Ankle Sprain?
2- Phase 1: Acute Phase and Post-Traumatic Inflammation Control (0-48h)
3- Phase 2: Recovery of Range of Motion and Activation (Subacute)
4- Phase 3: Reconditioning (Return to Play) and Functional Work
5- Phase 4: Return to Play and Performance
6- FAQ: Your Questions About Sprained Ankle Treatment
7- References
1- What is an Ankle Sprain?
An ankle sprain, and more specifically an injury to the lateral collateral ligament, generally occurs during a forced inversion movement. This trauma is never “just a twisted ankle.” It triggers a cascade of mechanical and sensorimotor consequences:
- Chronic Ankle Instability (CAI): Defined by a sensation of the ankle “giving way,” persistent apprehension, and frequent recurrences.
- Sensorimotor Deficit: The trauma disrupts communication between the joint and the central nervous system, requiring specific neuromuscular reprogramming.
- Risk of Osteoarthritis: A poorly rehabilitated ankle paves the way for early-onset osteoarthritis. In fact, 70% to 80% of ankle osteoarthritis cases are post-traumatic in origin.
The goal of modern rehabilitation is to break this cycle by relying on precise data to guide the patient from immediate post-trauma to peak performance.
2- Phase 1: Acute Phase and Post-Traumatic Inflammation Control (0-48h)
The primary objective of this initial stage is to break the cycle of pain and edema while protecting the healing tissues. During this phase, management is essentially focused on physical therapy and manual treatment.
Immediate Drainage and Analgesia
To combat the inflammatory process, dynamic cryocompression (such as the Game Ready system) is particularly effective. By lowering the skin temperature below 15°C, cold activates the gate control effect for long-lasting analgesia (3 to 6 hours). The associated dynamic compression promotes venous return and the evacuation of edema.
The Contribution of TECAR Therapy
In the clinic, TECAR therapy allows practitioners to go beyond passive treatment:
- Pushback Current: This specific current acts on the lymphovenous network and smooth muscles for deep drainage.
- Biological Effect: High frequency opens ion channels in cell membranes, stimulating the metabolic exchanges necessary for ligament healing.
- Pulse Analgesia (Lightens): This pulsed current combines the benefits of high-frequency stimulation with the endorphinic effect of low-frequency stimulation for immediate relief.
Objectifying Weight-Bearing with Kinvent

Even in the acute phase, it is crucial to verify the quality of weight-bearing and early muscle activation. Using connected force plates, such as K-Force Plates, allows you to:
- Quantify Weight-Bearing: Precisely monitor the percentage of body weight the patient can support without pain while weaning off crutches.
- Verify Early Activation: Ensure that the trauma has not already induced severe Arthrogenic Muscle Inhibition (AMI).
Transition Criteria to Phase 2: Controlled resting pain, stable or decreasing edema, and the ability to achieve at least partial weight-bearing.
3- Phase 2: Recovery of Range of Motion and Activation (Subacute)
Once resting pain is managed, the challenge is to restore joint function and reactivate the stabilizing muscle chains. This phase marks the beginning of active rehabilitation.
Restoring Range of Motion and Mobility
The priority is to regain correct mobility, which is essential for physiological gait and complex movements.
- Dorsiflexion: This is the most critical movement to recover to avoid compensations and recurrences. Criteria targets include an amplitude > 35° or > 10 cm on the Weight Bearing Lunge Test (WBLT). (Powden CJ et al. (2015) / Fousekis K et al. (2012)).
- Plantarflexion: Often overlooked, it is essential, particularly for the kneeling position (the “Seiza”). (Brockett CL & Chapman GJ (2016) / Rice H et al. (2024))
- Assessment with the Connected Goniometer (K-Move): Unlike traditional tools, it allows for the analysis of joint behavior. Beyond the maximum angle, practitioners can observe angular velocity and asymmetries in movement fluidity.
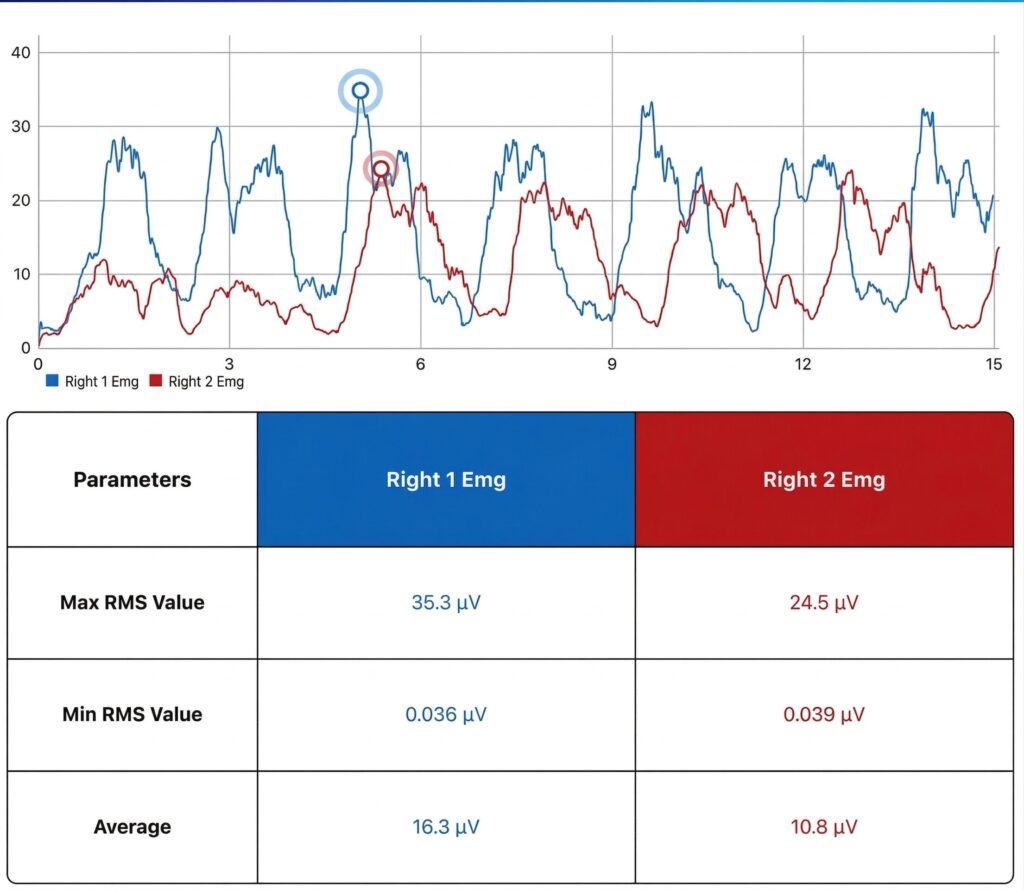
Overcoming Muscle Inhibition (AMI) through EMG
Following trauma, the brain often initiates Arthrogenic Muscle Inhibition (AMI). The patient may have difficulty voluntarily recruiting muscles like the peroneals or the soleus.
- Real-time feedback (K-Myo): The patient visualizes their muscle activation in real-time. This visual feedback facilitates neuromuscular reprogramming and motivates the patient by objectifying immediate progress.
- Results: This ensures the patient effectively activates the peroneals without excessive compensation from the dorsiflexors.
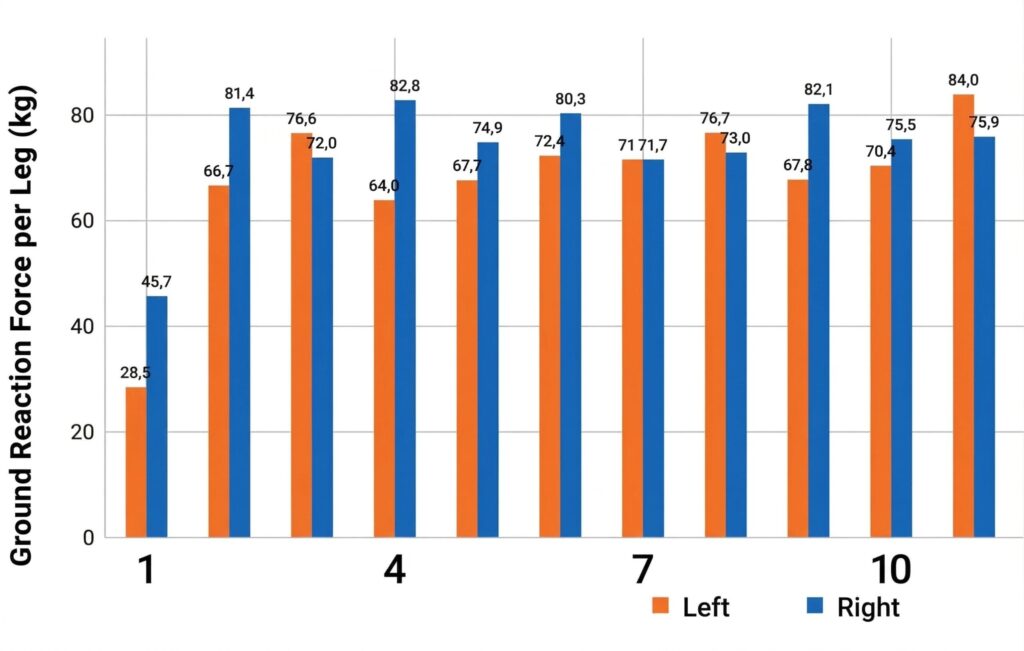
Postural Control and Bipedal Weight-Bearing
Before transitioning to full weight-bearing on one leg, force plates (e.g., K-Force Plates) are used to analyze static balance.
- Weight Distribution: Verify the symmetry of load between the healthy and injured leg.
- Balancing Strategies: Observe if the patient compensates by overloading the heel or if they successfully engage the forefoot and intrinsic muscles.
- Gamification: Using interactive games (e.g., moving a ball on the screen by shifting the center of pressure) helps lift psychological barriers and increases patient engagement.
Strength and Ratios with K-Push / K-Force Plates
Strengthening begins with isometric tests to objectify maximum strength deficits.
- Inverter/Everter Ratios: Evaluation allows for checking the agonist/antagonist balance of the ankle to prevent recurrences.
- Max Calf Strength: Assess the gastrocnemius (knee extended) and soleus (knee flexed) separately to detect strength asymmetries that might be missed during manual testing.
- Rate of Force Development (RFD): Practitioners begin monitoring how quickly the patient can produce force, a crucial indicator for future explosive phases.
Transition Criteria to Phase 3: Pain score < 3/10, a Limb Symmetry Index (LSI) for strength and stability < 20%, and a mobility deficit < 15% compared to the healthy side.
4- Phase 3: Reconditioning and Functional Work
This phase is the true engine of the recovery process. We shift from isolated ankle testing to analyzing the joint’s capacity to handle dynamic constraints, impact forces, and complex balance disruptions.
Mobility and Stability Under Load
- Weight-Bearing Lunge Test (WBLT): This is the “Gold Standard” for measuring functional dorsiflexion. We aim for perfect symmetry and, ideally, an amplitude > 35°.
- Y-Balance Test (YBT): This test evaluates dynamic stability. Particular attention is paid to the anterior reach: a difference of more than 4 cm compared to the healthy side is a major predictor of recurrence.
- Step Down Test: Here, we observe eccentric control and the stability of the hip-knee-ankle complex during a 19 cm step descent to detect any compensatory dynamic valgus.
Max Strength and Endurance (K-Push & K-Force Plates)
Strengthening becomes more intense and sport-specific:
- Heel Rise Test: This measures the endurance of the triceps surae. Success is defined as performing more than 25 repetitions with a full rise, without asymmetry in height or strategy between legs.
- Max Gastrocnemius and Soleus Strength: We isolate work with the knee extended (gastrocnemius) and knee flexed (soleus) using force plates to ensure no link in the posterior chain is deficient.
- Inverter/Everter Monitoring: We continue to monitor the strength ratio to ensure optimal lateral protection of the ankle.
Power and Impact Resumption
- Drop Landing (Bipedal & Unipodal): Analysis of jump landing. The K-Deltas force plates measure stabilization time and shock absorption capacity.
- Bipedal Counter Movement Jump (CMJ): We evaluate global explosiveness and thrust symmetry.
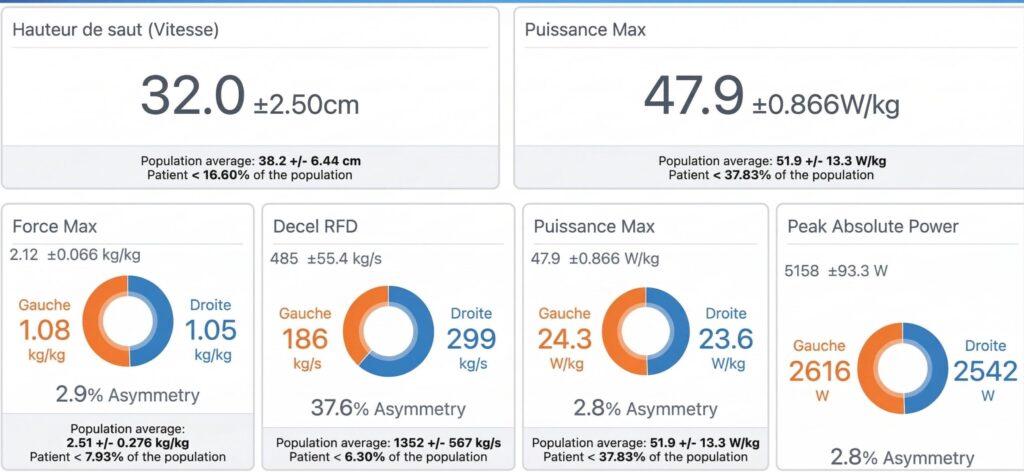
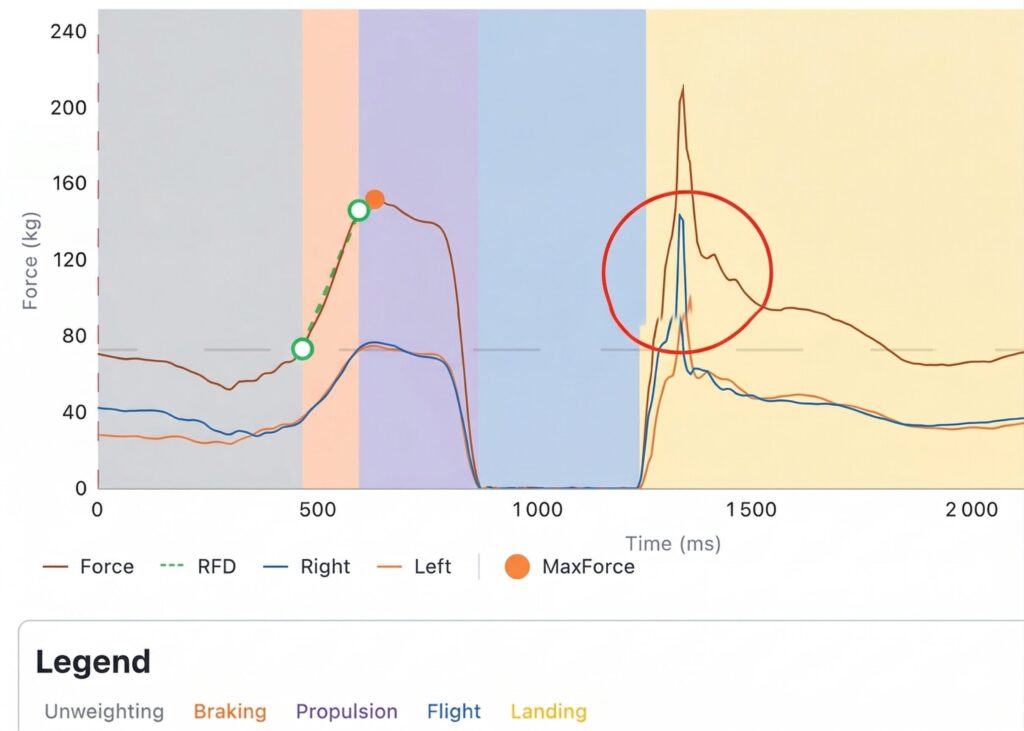
- Skipping (Return to Running): We validate the ability to perform low-level plyometrics (on-the-spot running simulation) with adequate ankle stiffness before authorizing a return to jogging.
Transition Criteria to the Final Phase:
To leave the reconditioning phase, the patient must validate these strict indicators:
- Pain: < 2/10 during dynamic testing.
- LSI (Limb Symmetry Index): ≤ 10% difference between limbs in strength and power.
- Mobility: Difference < 10% between sides and dorsiflexion angle > 35° (and < 4 cm difference on anterior YBT).
- Heel Rise Test: > 25 repetitions without asymmetry.
- Jumps: Jump landing and CMJ validated without avoidance strategies.
- Skipping: On-the-spot running and small hops validated without pain.
5- Phase 4: Return to Play and Performance
The final phase shifts from recovery to optimizing the athlete’s ability to withstand maximum sports-specific loads. The target is to reach a Limb Symmetry Index (LSI) of at least 90% (less than 10% asymmetry) to ensure a safe return to competition.
Advanced Mobility and Stability Monitoring
Mobility remains a critical safeguard even in the final stages of the protocol.
- Dorsiflexion & Plantarflexion: Final validation is performed through the Lunge Test and the “Seiza” position (Japanese sitting position) to confirm a full range of motion without impingement.
- Y-Balance Test (YBT): Confirms dynamic stability across all three axes.
- Single-Leg Eyes Closed (EC) Stability: This is the ultimate sensorimotor test; the patient should demonstrate a stable center of pressure (CoP) trace on the force plates without significant sway or “saccades”.
Comprehensive Strength Profiling
We verify the integrity of all muscle chains that stabilize the ankle and lower limb.
- Inverters & Everters: Evaluation of strength ratios to ensure optimal lateral protection against re-injury.
- Calf & Dorsiflexors: Validation via the Heel Rise Test (endurance) combined with isometric peak force measurements.
- Gluteus Medius: Strength at the hip is a major determinant in controlling chronic instability; a deficit here can compromise ankle stability during pivoting movements.
Functional Performance Tests (KPIs)
Performance is objectified by monitoring power, explosiveness, and agility.
- Drop (Hop) Landing: Unilateral landing analysis on force plates to measure stabilization time and shock absorption.
- Explosive Jumps:
- CMJ (Counter Movement Jump): Measures jump height and peak power.
- Drop Jump (15 cm): Used to calculate the RSI (Reactive Strength Index); a ratio > 1 indicates a functional “stiffness” ready for high-intensity running.
- 10/5 Jump: Evaluates plyometric ability and neuromuscular fatigue over repeated efforts.
- Agility & Change of Direction (COD):
- Modified Side Hop Test: Performed with a 30 cm distance to test medio-lateral stability under time pressure (14s).
- Figure-of-8 Test: Essential for validating rapid weight shifts and the patient’s psychological confidence in the joint (17s).
Video Analysis, 3D Performance, and VBT
For high-level athletes, we refine the movement through Velocity-Based Training (VBT). Using sensors like Kinvent’s K-Power on exercises such as Squats or Hip Thrusts ensures that execution speed remains optimal under load.

Additionally, 3D analysis coupled with video allows for the visualization of force vectors during pivots or changes of direction (COD). This technical approach facilitates the optimization of sports-specific movements by identifying compensations that are invisible to the naked eye.
Key performance tests include:
- Skater Jump
- Changement de Direction
- Broad Jump
- Single Hop Test
- Drop & Side Jump
- Modified Side Hop Test
Final Return to Play (RTP) Validation Criteria:
- Validated Scores: FAAM > 90%, Ankle-GO score, or ALR-RSI > 70 (psychological readiness).
- LSI (Limb Symmetry Index): < 10% across all strength and jump tests.
- Mobility: Deficit < 10% and dorsiflexion > 35°.
- Functional Mastery: Single-leg landings, single-leg CMJ, and Side Hops validated without pain or compensatory strategies.
6- FAQ: Your Questions About Sprained Ankle Treatment
How long does ankle sprain rehabilitation last?
There is no fixed timeframe, as every patient and injury is unique. While a return to sport is often discussed after 3 to 6 weeks, it must be validated by objective criteria for strength, mobility, and stability rather than a simple calendar date.
Why does my ankle still feel unstable?
Chronic Ankle Instability (CAI) is often linked to sensorimotor deficits or muscle inhibition. Using EMG (K-Myo) helps verify if stabilizing muscles (peroneals) activate at the right time or if there is a detrimental activation latency following the trauma.
When can I start weight-bearing exercises?
Weighted work (squats, lunges) can begin once pain levels are below 3/10 and bipedal weight-bearing is stable as measured on force plates.
What is the benefit of real-time feedback during exercises?
Immediate visual real-time feedback increases patient engagement and facilitates neuromuscular reprogramming. The patient better understands their deficits and can visualize their progress in real-time.
What is the Ankle-GO score?
It is a validated clinical tool designed to discriminate and predict return-to-sport outcomes specifically after a lateral ankle sprain.
7- References
- Aguilaniu A, Hardy A, Edouard P, et al. Current practice for safe return-to-play after lateral ankle sprain: A survey among French-speaking physicians. Foot Ankle Surg. 2022;28(4):496-502. doi: 10.1016/j.fas.2021.04.001
- Almansoof HS, Alsayed N, Alnasser N, et al. Role of ankle dorsiflexion in sports performance and injury risk: A narrative review. Eur J Gen Med. 2023;20(5):em531. doi: 10.29333/ejgm/13412
- Brockett CL, Chapman GJ. Biomechanics of the ankle. Orthop Trauma. 2016;30(3):232-238. doi: 10.1016/j.mporth.2016.04.015
- DeJong AF, Koldenhoven RM, Hertel J. Hip strength in patients with chronic ankle instability: A systematic review and meta-analysis. Phys Ther Sport. 2020;43:131-139. doi: 10.1016/j.ptsp.2020.02.013
- Delahunt E, Bleakley CM, Bossard DS, et al. Clinical assessment of acute lateral ankle sprain injuries (ROAST): 2019 consensus statement. Br J Sports Med. 2018;52(20):1304-1310. doi: 10.1136/bjsports-2017-099401
- Fousekis K, Tsepis E, Vagenas G. Intrinsic risk factors of noncontact ankle sprains in soccer: a prospective study on 100 professional players. Am J Sports Med. 2012;40(8):1842-1850. doi: 10.1177/0363546512449602
- Gabbe BJ, Bennell KL, Wajswelner H, Finch CF. Predictors of lower extremity injuries at the community level of Australian football. Clin J Sport Med. 2004;14(2):56-63. doi: 10.1097/00042752-200403000-00002
- Geerinck A, Salentey P, Lhermitte J, et al. French translation and validation of the Cumberland Ankle Instability Tool. Foot Ankle Surg. 2020;26(3):266-272. doi: 10.1016/j.fas.2019.03.004
- Hardy A, Edouard P, Gremeaux V, et al. The ALR-RSI scale for psychological readiness after ankle ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2020;28(9):2854-2860. doi: 10.1007/s00167-020-06020-6
- Hardy A, Picot B, Anract P, et al. Validation française de l’ALR-RSI. Journal of Experimental Orthopaedics. 2022;9(1):27. doi: 10.1186/s40634-022-00463-1
- Hébert-Losier K, Wessman C, Alricsson M, Svantesson U. Updated reliability and normative values for the standing heel-rise test in healthy adults. Physiotherapy. 2017;103(4):446-452. doi: 10.1016/j.physio.2017.03.002
- Hertel J. Sensorimotor Deficits with Ankle Sprains and Chronic Ankle Instability. Clin Sports Med. 2008;27(3):353-370. doi: 10.1016/j.csm.2008.03.004
- Hiller CE, Refshauge KM, Bundy AC, et al. The Cumberland ankle instability tool: validity and reliability. Arch Phys Med Rehabil. 2006;87(9):1235-1241. doi: 10.1016/j.apmr.2006.05.022
- Hou Y, Zhao J, Zhang Y. Characteristics and predictors of muscle strength deficit in mechanical ankle instability. BMC Musculoskelet Disord. 2020;21(1):602. doi: 10.1186/s12891-020-03468-4
- Khalaj N, Vicenzino B, Heales LJ, Smith MD. Is chronic ankle instability associated with impaired muscle strength? Ankle, knee and hip muscle strength in individuals with chronic ankle instability: a systematic review and meta-analysis. Br J Sports Med. 2020;54(14):839-847. doi: 10.1136/bjsports-2018-100070
- Kotsifaki A, Korakakis V, Whiteley R, et al. Measuring only hop distance during single leg hop testing is insufficient to detect deficits 9 months after ACL reconstruction. Br J Sports Med. 2021;55(20):1157-1163. doi: 10.1136/bjsports-2020-103684
- Lee M, Bubis E, Breckenridge B, et al. Normative isometric plantarflexion strength values for rugby athletes. Phys Ther Sport. 2023;61:166-171. doi: 10.1016/j.ptsp.2023.03.006
- Martin RL, Irrgang JJ, Burdett RG, et al. Evidence of validity for the Foot and Ankle Ability Measure (FAAM). Foot Ankle Int. 2005;26(11):968-983. doi: 10.1177/107110070502601113
- Mentiplay BF, Perraton LG, Bower KJ, et al. Assessment of Lower Limb Muscle Strength and Power Using Hand-Held and Fixed Dynamometry: A Reliability and Validity Study. PLoS ONE. 2015;10(10):e0140822. doi: 10.1371/journal.pone.0140822
- Picot B, Hardy A, Terrier R, et al. Which Functional Tests and Self-Reported Questionnaires Can Help Clinicians Make Valid Return to Sport Decisions in Patients With Chronic Ankle Instability? A Narrative Review and Expert Opinion. Frontiers in Sports and Active Living. 2022;4:902886. doi: 10.3389/fspor.2022.902886
- Picot B, Lopes R, Rauline G, et al. Development and Validation of the Ankle-GO Score for Discriminating and Predicting Return-to-Sport Outcomes After Lateral Ankle Sprain. Sports Health. 2024;16:47-57. doi: 10.1177/19417381231183647
- Picot B, Fourchet F, Lopes R, et al. Low Ankle-GO Score While Returning to Sport After Lateral Ankle Sprain Leads to a 9-fold Increased Risk of Recurrence: A Two-year Prospective Cohort Study. Sports Med Open. 2024;10:23. doi: 10.1186/s40798-024-00693-w
- Picot B, Fourchet F, Rauline G, et al. Ankle-GO score is associated with the probability of becoming coper after lateral ankle sprain: a 1-year prospective cohort study. Br J Sports Med. Publié en ligne le 9 août 2024. doi: 10.1136/bjsports-2024-108361
- Plisky PJ, Rauh MJ, Kaminski TW, Underwood FB. Star Excursion Balance Test as a predictor of lower extremity injury in high school basketball players. J Orthop Sports Phys Ther. 2006;36(6):436-446. doi: 10.2519/jospt.2006.2244
- Powden CJ, Hoch JM, Hoch MC. Reliability and minimal detectable change of the weight-bearing lunge test: A systematic review. Man Ther. 2015;20(4):524-532. doi: 10.1016/j.math.2015.01.010
- Powers CM, Ghoddosi N, Straub RK, Khayambashi K. Hip Strength as a Predictor of Ankle Sprains in Male Soccer Players: A Prospective Study. J Athl Train. 2017;52(11):1048-1055. doi: 10.4085/1062-6050-52.11.18
- Rabin A, Kozol Z, Spitzer E, Finestone AS. Limited ankle dorsiflexion increases the risk for mid-portion Achilles tendinopathy in infantry recruits: a prospective cohort study. J Foot Ankle Res. 2014;7:48. doi: 10.1186/s13047-014-0048-3
- Rice H, et al. Reliability of instrumented ankle plantarflexion testing using a fixed-frame dynamometer. Int J Sports Phys Ther. 2024;19(2):207-215. doi: 10.26603/001c.91664
- Russell JA, Hein J, Lamb T. Clinical assessment of the ankle: reliability of measures for dancers. J Dance Med Sci. 2010;14(3):98-103. PMID: 20831835
- Smith MD, Vicenzino B, Bahr R, et al. Return to sport decisions after an acute lateral ankle sprain injury: introducing the PAASS framework-an international multidisciplinary consensus. Br J Sports Med. 2021;55(22):1270-1276. doi: 10.1136/bjsports-2021-104087
- Tassignon B, Verschueren J, Delahunt E, et al. Criteria-Based Return to Sport Decision-Making Following Lateral Ankle Sprain Injury: a Systematic Review and Narrative Synthesis. Sports Med. 2019;49:601-19. doi: 10.1007/s40279-019-01071-3
- van Dijk CN. Anterior and posterior ankle impingement. Foot Ankle Clin. 2006;11(3):663-683. doi: 10.1016/j.fcl.2006.06.014
- Wikstrom EA, Mueller C, Cain MS. Lack of Consensus on Return-to-Sport Criteria Following Lateral Ankle Sprain: Systematic Review of Expert Opinions. J Sport Rehabil. 2020;29:231-7. doi: 10.1123/jsr.2019-0038